A hairline fracture, also known as a stress fracture, is a small crack in a bone that develops gradually due to repeated stress or overuse rather than a single traumatic injury. These types of fractures are common in athletes, runners, and individuals who suddenly increase their physical activity.
Unlike a complete bone break, a hairline fracture may start with mild discomfort that becomes progressively worse over time, especially during weight-bearing activities. Because the symptoms can be subtle at first, many people mistake it for muscle pain or general overuse.
Understanding what a hairline fracture is, what causes it, and how to recognize the early signs is essential for preventing further damage and ensuring proper healing.
Key Clinical Points – Hairline (Stress) Fracture
- Hairline (stress) fracture is a small crack in a bone caused by repetitive stress and overuse rather than a single traumatic injury.
- It most commonly affects weight-bearing bones such as the foot, tibia (shin), femoral neck (hip), and navicular bone.
- These injuries are frequent in athletes, runners, and individuals with sudden increases in physical activity or training intensity.
- Symptoms usually begin gradually with mild pain during activity that worsens over time and may persist at rest in advanced cases.
- Early diagnosis can be challenging, as initial X-rays may appear normal; MRI is the most sensitive imaging method for detection.
- Treatment focuses on rest, activity modification, and gradual rehabilitation to allow proper bone healing and prevent progression.
- If left untreated, stress fractures can progress into a complete fracture and lead to prolonged recovery and complications.
What Is a Hairline Fracture?
A hairline fracture, also known as a stress fracture, is a small crack in a bone that develops gradually, most often due to repeated stress rather than a single injury. Unlike a complete fracture, the bone does not break entirely, which is why symptoms can be subtle in the beginning.
These fractures are often overlooked or misdiagnosed because the pain typically starts as mild and appears only during activity. Many people confuse it with muscle soreness or overuse, especially in the early stages. Additionally, hairline fractures may not always be visible on initial X-rays, making early detection more challenging.
Although they can affect anyone, hairline fractures are most commonly seen in people who put repeated strain on their bones, particularly in weight-bearing areas like the legs and feet.
How Does a Hairline Fracture Occur?
A hairline fracture develops when a bone is exposed to repetitive stress over time without enough opportunity to recover. Bones are living tissues that constantly adapt to physical load, but when the stress placed on them exceeds their ability to repair, small cracks can begin to form.
This is what distinguishes stress fractures from acute fractures. Acute fractures usually result from a sudden, high-impact injury—such as a fall or direct blow—causing the bone to break immediately. In contrast, a hairline fracture forms gradually, often without a clear moment of injury, making it harder to recognize early.
Overuse and insufficient recovery play a key role in this process. Activities like running, jumping, or prolonged walking can repeatedly load the same areas of bone. If rest periods are too short or training intensity increases too quickly, the body cannot keep up with the repair process. Over time, this imbalance between stress and recovery leads to the development of a hairline fracture.
Common Causes and Risk Factors
Hairline fractures are typically the result of repeated stress on the bones combined with insufficient recovery. While they can develop in anyone, certain habits and conditions significantly increase the risk.
The most common causes include a sudden increase in physical activity, especially when the body is not given enough time to adapt. High-impact sports such as running, basketball, and dancing place continuous load on weight-bearing bones, making them particularly vulnerable. Training on hard surfaces or wearing improper footwear can further amplify this stress by reducing shock absorption.
In addition to mechanical factors, internal conditions also play an important role. Low bone density weakens the structure of bones, making them more prone to small cracks. Nutritional deficiencies—especially inadequate intake of calcium and vitamin D—can impair bone strength and recovery. Hormonal imbalances may also affect bone metabolism, increasing susceptibility to stress injuries.
A specific condition known as the Female Athlete Triad—which includes low energy availability, menstrual dysfunction, and decreased bone density—significantly increases the risk of stress fractures, particularly in physically active women.
Key risk factors include:
- Sudden increase in training intensity or duration
- Participation in high-impact sports
- Poor footwear or hard training surfaces
- Low bone density
- Calcium and vitamin D deficiency
- Hormonal imbalances
- Female Athlete Triad
Understanding these factors is essential for both prevention and early recognition of a hairline fracture.
Hairline Fracture Symptoms
The symptoms of a hairline fracture often develop gradually, which is why they are easy to overlook in the early stages. The pain typically starts as mild and intermittent but becomes more noticeable as the injury progresses.
One of the most common signs is localized pain that worsens with physical activity, especially movements that put stress on the affected bone. At first, the discomfort may disappear with rest, but in more advanced cases, the pain can persist even when you are not active.
You may also notice tenderness when pressing on a specific area, along with mild swelling. As the condition worsens, everyday movements such as walking or standing can become uncomfortable, leading to difficulty bearing weight or even a noticeable limp.
Common symptoms include:
- Localized pain that increases with activity
- Pain that may persist at rest (in later stages)
- Tenderness in a specific area
- Mild swelling
- Difficulty bearing weight or limping
Recognizing these symptoms early can help prevent the injury from progressing into a more serious fracture.
Most Common Locations
Hairline fractures (stress fractures) most often occur in weight-bearing bones that are repeatedly exposed to load and impact. Their frequency depends on biomechanics, training patterns, and the amount of stress placed on each region.
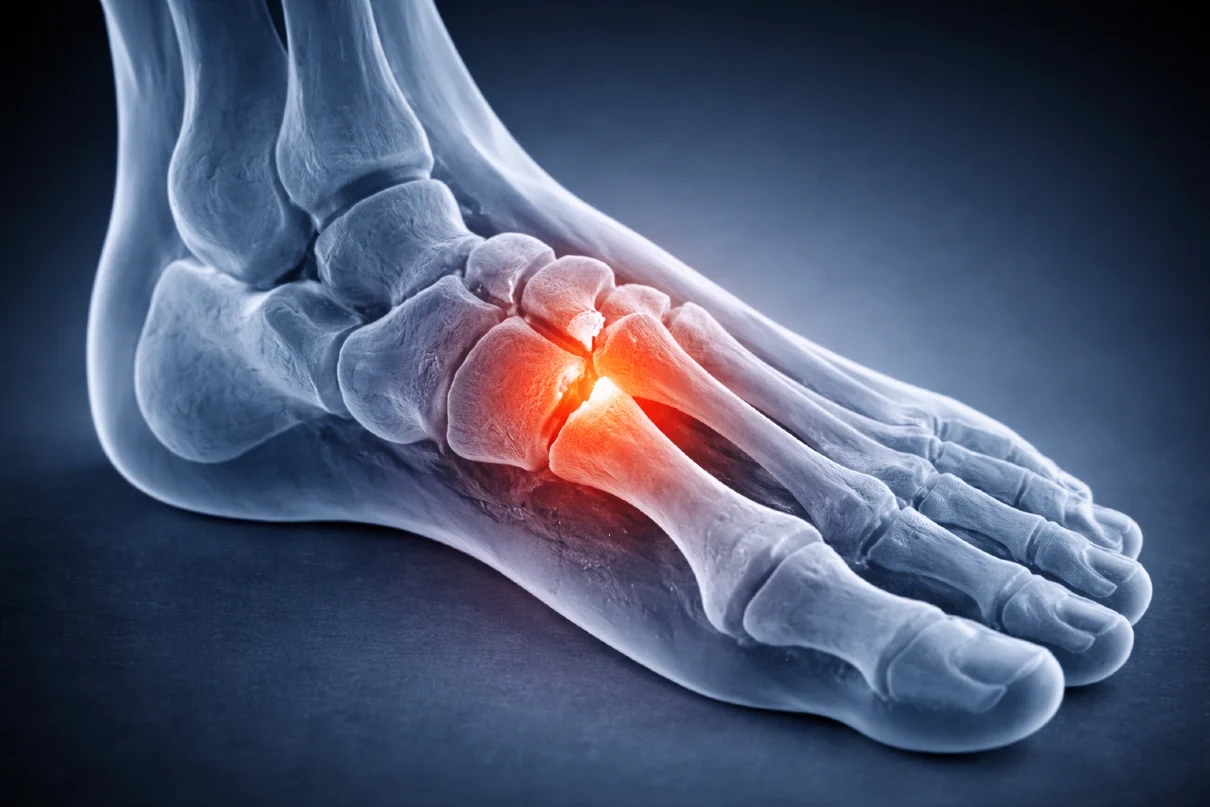
1. Metatarsals (Foot)
The metatarsal bones are the most common site of hairline fractures. They absorb repeated impact during walking and running, making them especially vulnerable in runners and active individuals. Sudden increases in training volume or intensity are a typical trigger.
2. Navicular Bone (Midfoot)
The navicular bone is another frequent location, particularly in athletes involved in sprinting, jumping, and sports with high repetitive loading. Navicular stress fractures are often more difficult to detect early and may present with vague midfoot pain.
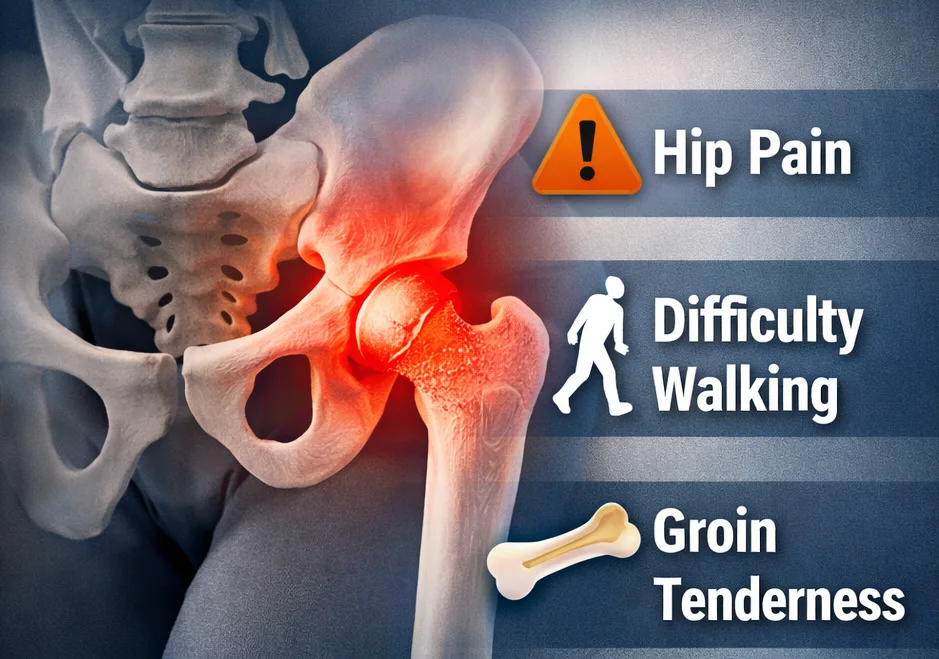
3. Femoral Neck (Hip)
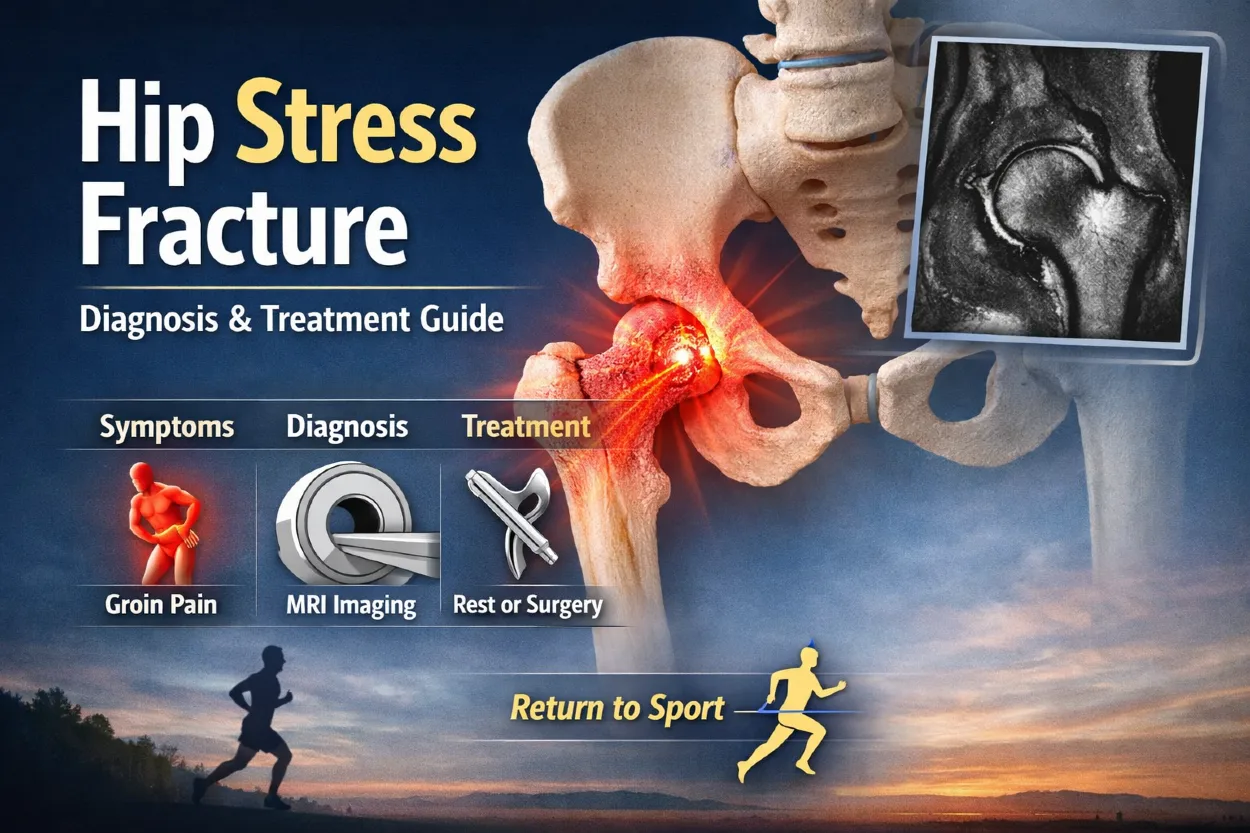
The femoral neck is a clinically important site of stress fractures, especially in endurance athletes and individuals with low bone density. These fractures are serious because they affect hip stability and may significantly limit weight-bearing activity.
Learn more about symptoms, causes, diagnosis, and recovery options in our detailed guide: Hip Stress Fracture – Complete Guide
4. Tibia (Shin)
The tibia is commonly affected in runners and individuals engaged in high-impact sports. Repetitive loading leads to microdamage along the bone, often presenting as pain along the inner shin (commonly referred to as shin splints in early stages).
5. Lumbar Spine (Lower Back)
Stress fractures in the lumbar spine (often pars interarticularis) — is also called spondylolysis. They are more common in sports involving repeated spinal extension and rotation, such as gymnastics, weightlifting, and some field sports. Symptoms may be subtle and mistaken for muscle strain.
Learn more about symptoms, causes, diagnosis, and treatment options in our detailed guide: Spondylolysis – Complete Guide
Diagnosis: How To Detect Hairline Fracture?
Diagnosing a hairline fracture can be challenging because symptoms often develop gradually and may resemble other overuse injuries. A proper diagnosis usually combines clinical evaluation with imaging techniques.
Physical examination is typically the first step. A healthcare professional will assess the painful area, check for localized tenderness, swelling, and evaluate how the pain responds to movement or pressure. They will also ask about recent changes in activity level, training intensity, or repetitive stress.
One of the main challenges is that X-rays may not show early hairline fractures. In the initial stages, the crack in the bone is often too small to be visible on standard radiographs. This is why patients may initially receive a normal X-ray result despite ongoing symptoms.
For more accurate detection, advanced imaging is often required. MRI scans are considered the most sensitive method because they can detect early bone stress reactions before a visible fracture develops. Bone scans can also be useful, as they highlight areas of increased bone activity associated with stress injury.
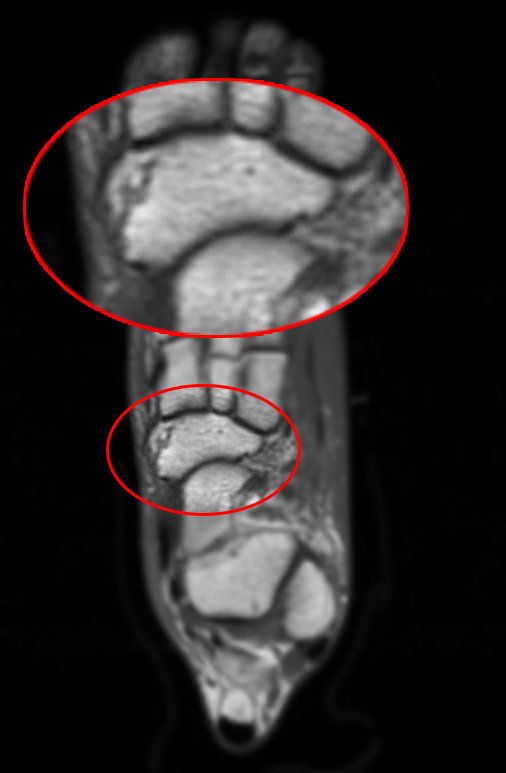
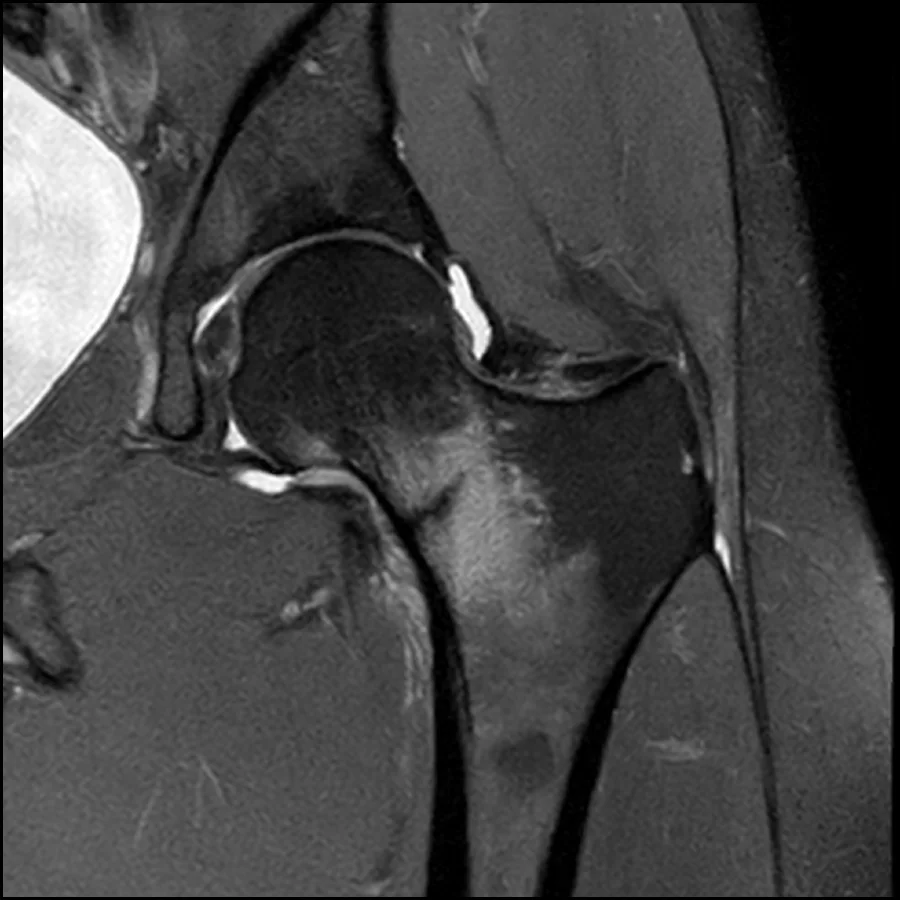
It is important to seek medical evaluation if pain persists, worsens with activity, or interferes with normal movement. Early assessment helps prevent progression into a more serious fracture and allows for faster recovery.
Treatment and Recovery
Treatment of a stress fracture focuses primarily on allowing the bone to heal while preventing further stress to the affected area. Early management is essential to avoid progression into a complete fracture.
The first and most important step is rest and activity modification. This means reducing or completely stopping activities that place load on the injured bone, such as running, jumping, or prolonged walking. In some cases, low-impact activities may be allowed depending on the severity and location of the injury.
For more significant fractures or high-risk areas, immobilization may be required. This can include the use of a walking boot, brace, or, in certain cases, crutches to completely offload the affected bone and promote healing.
Once pain begins to improve, physical therapy is often introduced. Rehabilitation focuses on restoring strength, improving biomechanics, and correcting any movement patterns that may have contributed to the injury.
A gradual return to activity is crucial. Returning too quickly can lead to reinjury, so activity levels are typically increased step by step under professional guidance.
Recovery timelines vary depending on the bone involved, severity of the fracture, and overall health. In general, healing can take anywhere from 6 to 12 weeks, although some stress fractures—especially in high-risk areas like the femoral neck—may require a longer recovery period.
What Happens If It’s Left Untreated?
A hairline fracture is not a condition that resolves on its own if the underlying stress continues. Without proper rest and management, the injury can progressively worsen and lead to more serious complications.
One of the most significant risks is progression to a complete fracture. Continued loading on an already weakened bone can cause the small crack to expand, resulting in a full break that may require more complex treatment and significantly longer recovery.
If left untreated, patients may also develop chronic pain and long-term complications. Persistent stress on the injured area can lead to ongoing inflammation, reduced bone strength, and in some cases, structural changes that affect normal movement patterns.
Another important consequence is increased recovery time. What could have been a relatively straightforward healing process of several weeks may turn into a prolonged rehabilitation period lasting months, particularly if the injury worsens or spreads to a higher-risk fracture site.
For these reasons, early recognition and appropriate management are essential to prevent escalation and ensure optimal healing outcomes.
Prevention Tips
Hairline fractures are largely preventable when training load, recovery, and bone health are properly managed. The goal is to reduce repetitive stress on the skeleton while allowing adequate adaptation over time.
Prevention Tips for Hairline Fractures
- Gradual progression in training: Increase training load slowly to allow bones and tissues to adapt and avoid overload.
- Proper footwear: Wear supportive shoes with adequate cushioning to reduce impact stress on the lower limbs.
- Strength training and conditioning: Build muscular strength to improve shock absorption and reduce direct bone stress.
- Balanced nutrition: Ensure sufficient intake of calcium, vitamin D, and protein to support bone health and remodeling.
- Rest and recovery: Include regular rest days to allow micro-damage in bone tissue to repair properly.
When to See a Doctor
It is important to seek medical evaluation if you suspect a hairline fracture, as early diagnosis can prevent the injury from worsening.
You should see a doctor if:
- Pain lasts more than a few days and does not improve with rest
- Pain occurs during normal daily activities such as walking or standing
- You are unable to fully bear weight on the affected limb
These signs may indicate a stress injury that requires proper assessment and imaging to confirm the diagnosis and guide treatment.
Conclusion
Hairline fractures are often subtle injuries that can easily be mistaken for minor muscle pain or overuse, which is why early recognition is essential. Identifying symptoms at an early stage allows for timely treatment and significantly reduces the risk of complications.
It is important to listen to your body. Persistent or activity-related pain should never be ignored, especially when it gradually worsens over time or begins to affect daily movement. Rest and proper evaluation are key to preventing further damage.
In summary, hairline fractures develop from repetitive stress, present with gradually increasing pain, and require early diagnosis and appropriate rest for full recovery. Awareness and early action are the most effective tools in ensuring a safe and complete healing process.
Kahanov L et al. Diagnosis, treatment, and rehabilitation of stress fractures in the lower extremity in runners. Open Access J Sports Med. PubMed: Stress fractures in runners – diagnosis and rehabilitation
May T, Marappa-Ganeshan R. Stress Fractures. StatPearls Publishing. StatPearls: Evidence-based overview of stress fractures
Bergman R, Kaiser K. Stress Reaction and Fractures. StatPearls Publishing. StatPearls: Stress reaction and fracture clinical review
da Rocha Lemos Costa TM et al. Stress fractures. Archives of Endocrinology and Metabolism. PubMed: Pathophysiology and management of stress fractures
Paavana T et al. Stress fractures of the foot – current evidence on management. Journal of Clinical Orthopaedics and Trauma. PubMed: Current evidence on foot stress fracture management
British Journal of Sports Medicine. International Delphi consensus on bone stress injuries in athletes. BJSM: Consensus guidelines for bone stress injuries in athletes
Robinson PG et al. Stress fractures: diagnosis and management in the primary care setting. British Journal of General Practice. BJGP: Primary care approach to stress fracture diagnosis and management