Hip pain can range from a mild annoyance to something that disrupts your daily life—making it harder to walk, sleep, or even sit comfortably. One of the most common causes of pain on the outside of the hip is bursitis, but it’s often mistaken for other conditions like muscle strain or arthritis. That’s why understanding how to tell if your hip pain is bursitis is key to getting the right treatment and avoiding long-term discomfort.
In this guide, we’ll break down the most common symptoms of hip bursitis, how it differs from other types of hip pain, and what steps you can take to confirm a diagnosis. Whether your pain started suddenly or has been building over time, recognizing the signs early can help you take control and recover faster.
Key Facts – How to Recognize Hip Bursitis
- Outer hip pain is the key sign – hip bursitis typically causes pain on the outside of the hip, not deep in the groin.
- Pain worsens with pressure – discomfort is often triggered when lying on the affected side or pressing on the outer hip.
- Pain increases with movement – walking, climbing stairs, or standing up from sitting often makes symptoms worse.
- Tenderness over the outer hip – the area may feel sore or sensitive even to light touch.
- Night pain is common – many people notice worsening pain when lying in bed on the affected side.
- Radiation pattern helps differentiate – pain may travel down the thigh but usually stays above the knee, unlike sciatica.
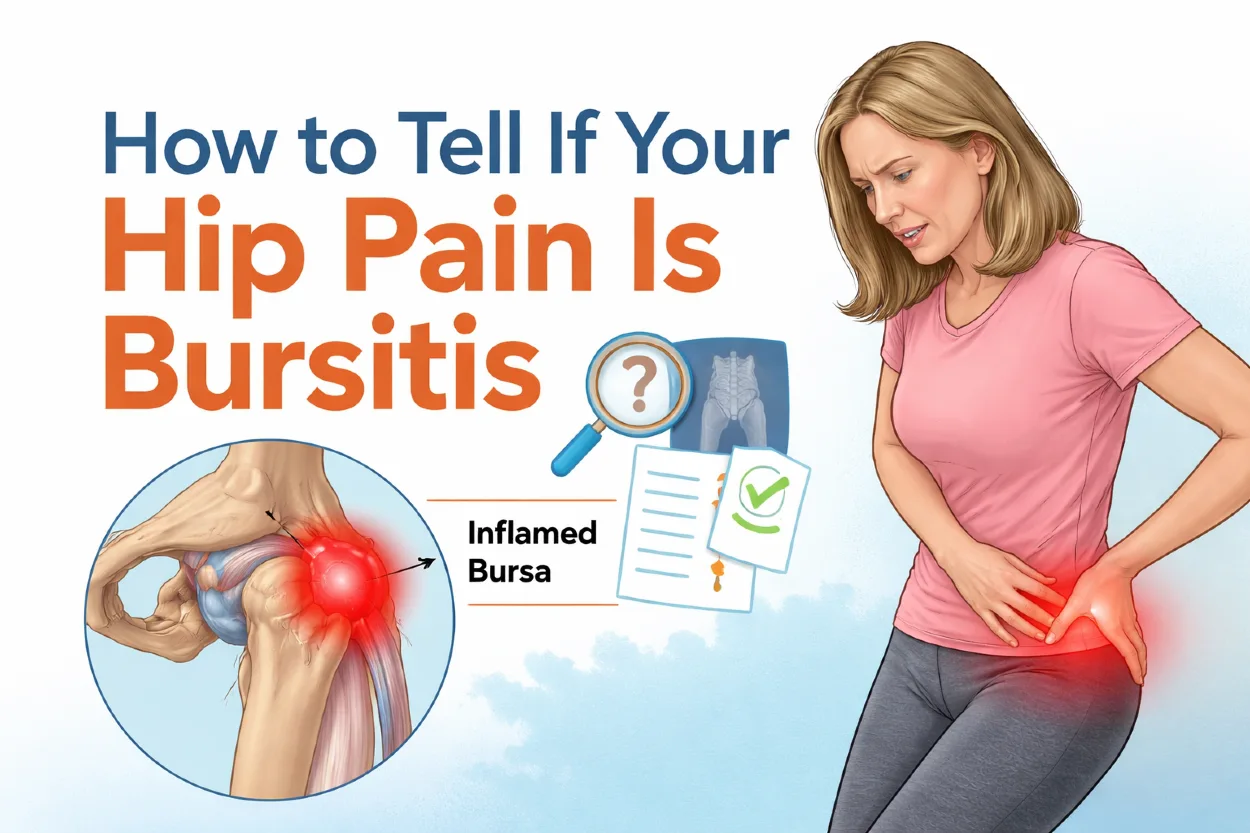
What Is Hip Bursitis?
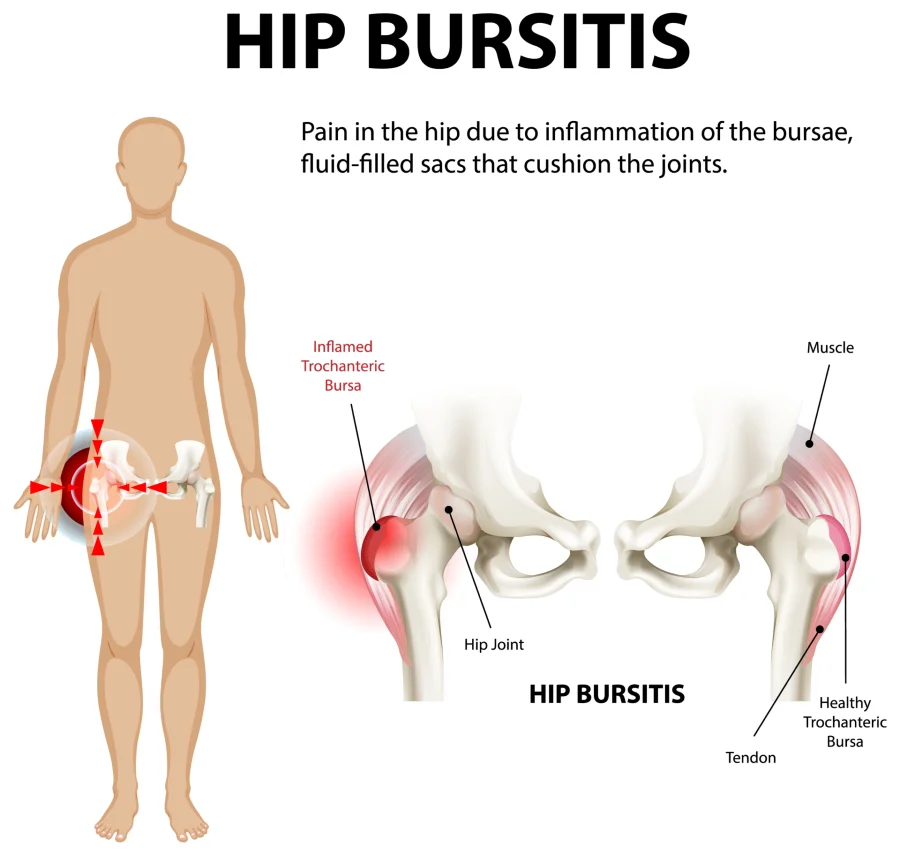
Hip bursitis is a condition that occurs when one of the small, fluid-filled sacs called bursae becomes inflamed. These bursae are located around your hip joint and act as cushions, reducing friction between bones, tendons, and muscles during movement.
The hip contains several bursae, but the one most commonly affected is located on the outer side of the hip, near a bony point called the greater trochanter. When this bursa becomes irritated or inflamed, the condition is often referred to as trochanteric bursitis.
Inflammation can develop gradually due to repetitive movements like walking, running, or cycling, or it can happen suddenly after an injury or prolonged pressure on the hip—such as lying on one side for extended periods. As the bursa becomes inflamed, it can cause pain, tenderness, and stiffness, especially during movement or when pressure is applied to the area.
Although hip bursitis is usually not serious, it can become persistent if left untreated. Understanding what it is and how it develops is the first step toward recognizing the symptoms and managing the condition effectively.
How to Tell If Your Hip Pain Is Bursitis: Key Signs
Hip bursitis is often misdiagnosed as hip osteoarthritis or sciatica, which can delay proper diagnosis and treatment. Recognizing bursitis early can make a big difference in how quickly you recover and how well you manage the pain. While symptoms can vary from person to person, there are several clear signs that point specifically to hip bursitis.
1. Pain on the Outside of the Hip
The most characteristic symptom is pain located on the outer side of the hip, rather than deep in the groin. This pain often starts as sharp and intense, especially during movement or after activity, and may gradually turn into a more constant, dull ache over time.
2. Pain When Lying on One Side
Discomfort that worsens when lying on the affected side—particularly at night—is a classic sign of hip bursitis. Many people find it difficult to sleep on that side due to direct pressure on the inflamed bursa.
3. Tenderness to Touch
The outer hip may feel sore or sensitive when pressed. Even light touch or pressure, such as from tight clothing or sitting against a hard surface, can trigger noticeable discomfort.
4. Pain That Worsens with Movement
Certain everyday activities tend to aggravate bursitis-related pain, including walking, climbing stairs, or standing up after sitting. Repetitive movements or prolonged activity can make symptoms more noticeable.
5. Stiffness After Rest
You may experience stiffness in the hip after periods of inactivity, such as sitting or lying down for a long time. This stiffness is often most noticeable when you first get up and start moving again, but it usually eases slightly as you loosen up.
These symptoms typically develop gradually, although they can also appear suddenly after an injury or overuse. If your pain matches this pattern—especially if it’s focused on the outer hip and worsens with pressure or movement—bursitis is a likely cause.
What Causes Hip Bursitis?
Hip bursitis most commonly develops due to a combination of mechanical overload, muscle imbalance, and prolonged irritation of the tissues around the hip—rather than a single isolated cause. It is closely linked to what is often described as greater trochanteric pain syndrome (GTPS), where both the bursa and surrounding tendons are involved.
Several key factors can contribute to its development:
- Repetitive stress and overuse – Activities like running, long-distance walking, or cycling can overload the lateral hip structures, especially without adequate recovery.
- Gluteal muscle weakness or imbalance – Weak hip stabilizers (particularly the gluteus medius and minimus) can increase strain on the bursa and surrounding tendons.
- Prolonged compression of the hip – Frequently lying on one side or sitting with legs crossed can compress the outer hip and irritate the bursa over time.
- Poor movement mechanics – Abnormal gait patterns, pelvic instability, or poor posture can create uneven load distribution across the hip.
- Direct trauma – A fall or direct blow to the outer hip can trigger inflammation.
- Underlying conditions – Issues such as hip osteoarthritis, lower back problems, or leg length differences can increase stress on the hip and contribute to bursitis.
In many cases, hip bursitis is not just inflammation of the bursa alone, but part of a broader dysfunction in how the hip moves and handles load. That’s why addressing the root cause—rather than just the pain—is key to long-term relief.
Hip Bursitis vs. Other Hip Pain: How to Tell the Difference
Not all hip pain is caused by bursitis, and distinguishing between different conditions is key to getting the right treatment. While symptoms can overlap, there are some important differences to look out for.
- Hip arthritis: Pain is typically felt deeper in the joint or in the groin area, rather than on the outer hip. It is often accompanied by stiffness, especially in the morning or after inactivity, and may limit your range of motion over time. In contract, range of motion is usually normal in hip bursitis.
- Muscle strain: This type of pain usually follows a specific injury or sudden movement. It tends to improve with rest and gradually resolves as the muscle heals. In contrast hip bursitis symptoms tend to last for weeks, even months.
- Sciatica: Pain from sciatica often starts in the lower back or buttock and radiates down the leg. It may be accompanied by tingling, numbness, or a burning sensation. Pain from hip bursitis can sometimes radiate down the leg, but it usually stays above the knee. In contrast, sciatica pain more commonly travels below the knee and can be felt in the calf, ankle, or foot.
If your pain is clearly localized on the outside of the hip and worsens with pressure (such as lying on that side) or with movement, bursitis is a more likely cause.
Clinical Insight
If your pain is clearly localized on the outside of the hip and worsens with pressure (such as lying on that side) or with movement, hip bursitis is a more likely cause.
| Condition | Main Pain Location | Key Characteristics | Typical Pattern |
|---|---|---|---|
| Hip Bursitis | Outer side of the hip | Tender to touch, pain when lying on affected side, worsens with movement or pressure | Localized, activity-related pain |
| Hip Arthritis | Deep in the hip or groin | Stiffness, reduced range of motion, gradual worsening over time | Chronic pain with morning stiffness |
| Muscle Strain | Specific muscle area around hip or thigh | Usually follows injury or overuse, improves with rest | Acute pain that resolves with recovery |
| Sciatica | Lower back, buttock, and down the leg | Radiating pain, tingling, numbness, or burning sensation | Nerve-related, radiating pattern |
When Should You See a Doctor?
While mild bursitis can often improve on its own, you should seek medical attention if:
- Pain lasts longer than a few weeks
- It becomes severe or starts limiting your mobility
- You notice swelling, redness, or warmth around the hip
- Over-the-counter pain relief does not help
How to Treat Hip Bursitis
Most cases of hip bursitis (often part of greater trochanteric pain syndrome) can be effectively managed without surgery. The main goal of treatment is to reduce irritation of the bursa, improve hip load tolerance, and correct contributing movement or strength issues.
Rest and Activity Modification
Avoid activities that worsen pain, especially repetitive impact movements like running or long walks. It’s also important to reduce prolonged pressure on the affected side, such as lying on the painful hip.
Ice and Symptom Relief
Ice packs can help reduce pain and inflammation, particularly after activity. Short-term use of anti-inflammatory medications may also help manage symptoms during flare-ups.
Physical Therapy Exercises
Targeted exercise therapy is one of the most important parts of recovery. Strengthening the gluteal muscles (especially gluteus medius) helps improve hip stability and reduce stress on the bursa. A structured rehab program also focuses on correcting movement patterns and improving load distribution.
Corticosteroid Injections
In cases where pain persists despite conservative treatment, corticosteroid injections may be used to reduce inflammation and provide short-term relief, allowing rehabilitation exercises to progress more effectively.
Long-Term Management
Addressing underlying factors such as poor biomechanics, muscle weakness, or training errors is key to preventing recurrence. Gradual return to activity and consistent strengthening exercises significantly improve long-term outcomes.
Final Thoughts
Hip bursitis is a common but often misunderstood cause of outer hip pain, and it is frequently confused with conditions like osteoarthritis or sciatica. Because of this overlap, diagnosis can sometimes be delayed, leading to prolonged discomfort and frustration.
The good news is that most cases respond well to conservative treatment, especially when addressed early. Rest, activity modification, and a focused rehabilitation program that improves hip strength and movement control are usually key to recovery. In more persistent cases, additional medical treatments can help reduce inflammation and support healing.
Understanding the difference between bursitis and other types of hip pain is essential for choosing the right approach. If symptoms persist or worsen, a proper medical evaluation is important to confirm the diagnosis and rule out other underlying conditions.
Pumarejo Gómez L, Li D, Childress JM. Greater Trochanteric Pain Syndrome (Greater Trochanteric Bursitis). StatPearls Publishing (Updated 2024). StatPearls: Greater Trochanteric Pain Syndrome overview
Speers CJ, Bhogal GS. Greater trochanteric pain syndrome: a review of diagnosis and management in general practice. Br J Gen Pract. 2017. BJGP review: Diagnosis and management of GTPS
BMJ Best Practice. Greater trochanteric pain syndrome. BMJ clinical guide: GTPS diagnosis and treatment
BMJ (2009). Comparison of fluoroscopically guided and blind corticosteroid injections for greater trochanteric pain syndrome. BMJ study: Corticosteroid injection outcomes in GTPS
BMJ Rapid Response. Trochanteric bursitis: diagnosis and injection therapy considerations. Clinical discussion: Trochanteric bursitis injection approach
StatPearls. Hip Bursitis. NCBI Bookshelf. Evidence-based overview: Hip bursitis pathophysiology and management