Dry needling is a modern therapeutic technique that uses thin, solid filiform needles to target myofascial trigger points, reduce pain, and restore normal muscle function. It is considered a minimally invasive procedure and has become increasingly relevant in the treatment of musculoskeletal pain and movement dysfunction.
As a specialist in Physical Medicine and Rehabilitation, I understand the growing interest in evidence‑based interventions that directly address the source of pain. Dry needling has gained significant attention because it offers a precise, targeted approach that can meaningfully improve quality of life for patients struggling with persistent muscle‑related symptoms.
In this article, we will clearly define what dry needling is, explain how it works, and outline the clinical situations in which it can be beneficial. Whether you are already familiar with this technique or exploring new treatment options, the goal is to provide a clear, medically grounded overview
What Is Dry Needling?
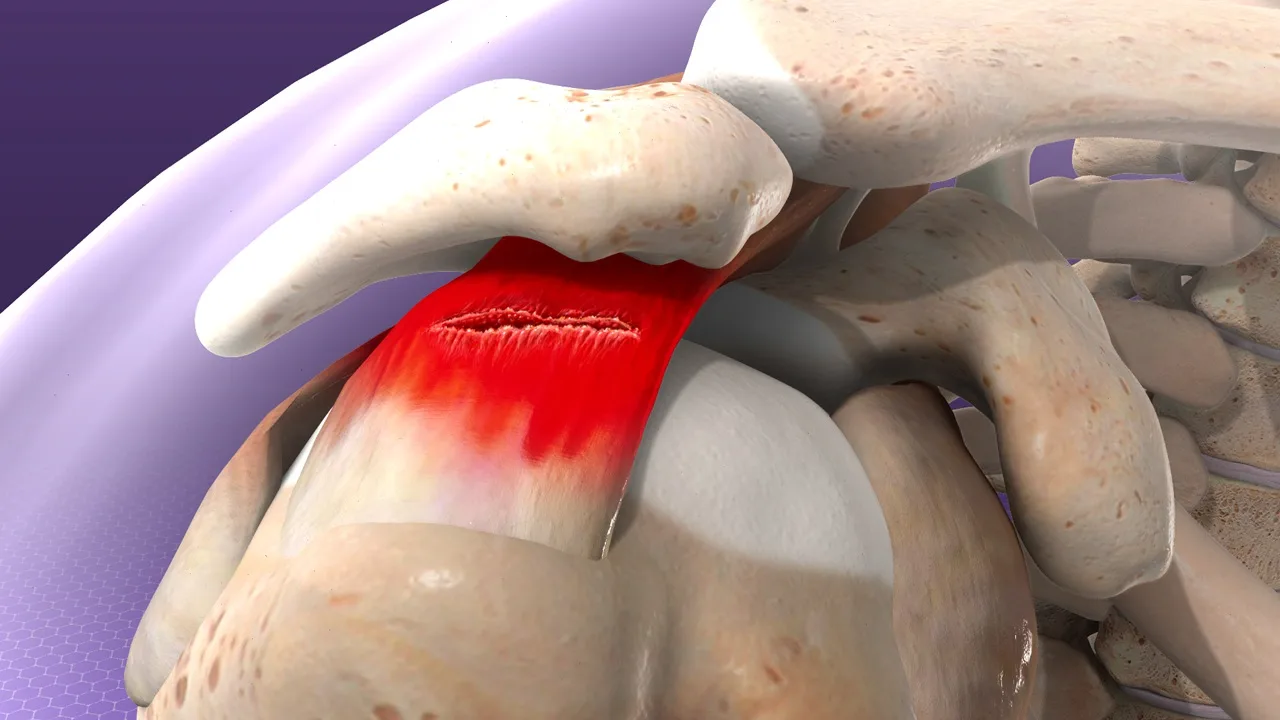
Dry needling is a therapeutic procedure used to treat pain and movement dysfunction by inserting a thin, sterile filiform needle through the skin to stimulate specific tissues. These targets typically include myofascial trigger points, connective tissue, and dysfunctional muscle fibers. The technique aims to reduce pain, normalize muscle tone, and restore healthy movement patterns.
Although dry needling uses the same type of needles as acupuncture, it is considered a distinct clinical approach based on Western medical science, anatomy, and neurophysiology. A more detailed comparison between dry needling and acupuncture will be discussed later in the article.
A Brief History of Dry Needling
The development of dry needling dates back to the early 20th century, when clinicians first began inserting needles into painful muscle areas while injecting local anesthetics. Over time, it became clear that the analgesic effect was the same even without the anesthetic. By the late 1970s, this observation led to the adoption of the term “dry needling”, referring to the use of a dry (non‑injecting) needle to treat pain and muscle dysfunction.
Throughout the following decades, the technique continued to evolve as research on myofascial trigger points, neuromuscular physiology, and pain mechanisms expanded. In the 21st century, dry needling gained significant global popularity, particularly among physiatrists, physical therapists, and sports medicine clinicians, as evidence increasingly supported its role in managing myofascial pain, movement dysfunction, and neuromuscular imbalance.
Today, dry needling is recognized as a modern, evidence‑informed intervention that integrates anatomical knowledge, clinical reasoning, and precise needle application — forming an important component of contemporary musculoskeletal rehabilitation.
What Are Trigger Points?
Trigger points are hyper‑irritable spots found within a taut band of skeletal muscle. These points become painful when pressed, stretched, overloaded, or when the muscle contracts. A key characteristic of trigger points is that they often produce referred pain — discomfort felt at a location distant from the actual source of the problem.
For example, trigger points in the muscles around the shoulder blade can cause pain that radiates into the neck, head, or down the arm. Similarly, trigger points in the cervical muscles may refer pain into the head, sometimes mimicking a migraine‑like pattern. These are only a few examples; referred pain patterns from trigger points are well‑documented and can vary widely depending on the muscle involved.
Trigger points are a central focus of dry needling therapy because targeting them with a fine needle can help reduce local sensitivity, interrupt pain pathways, and restore normal muscle function.
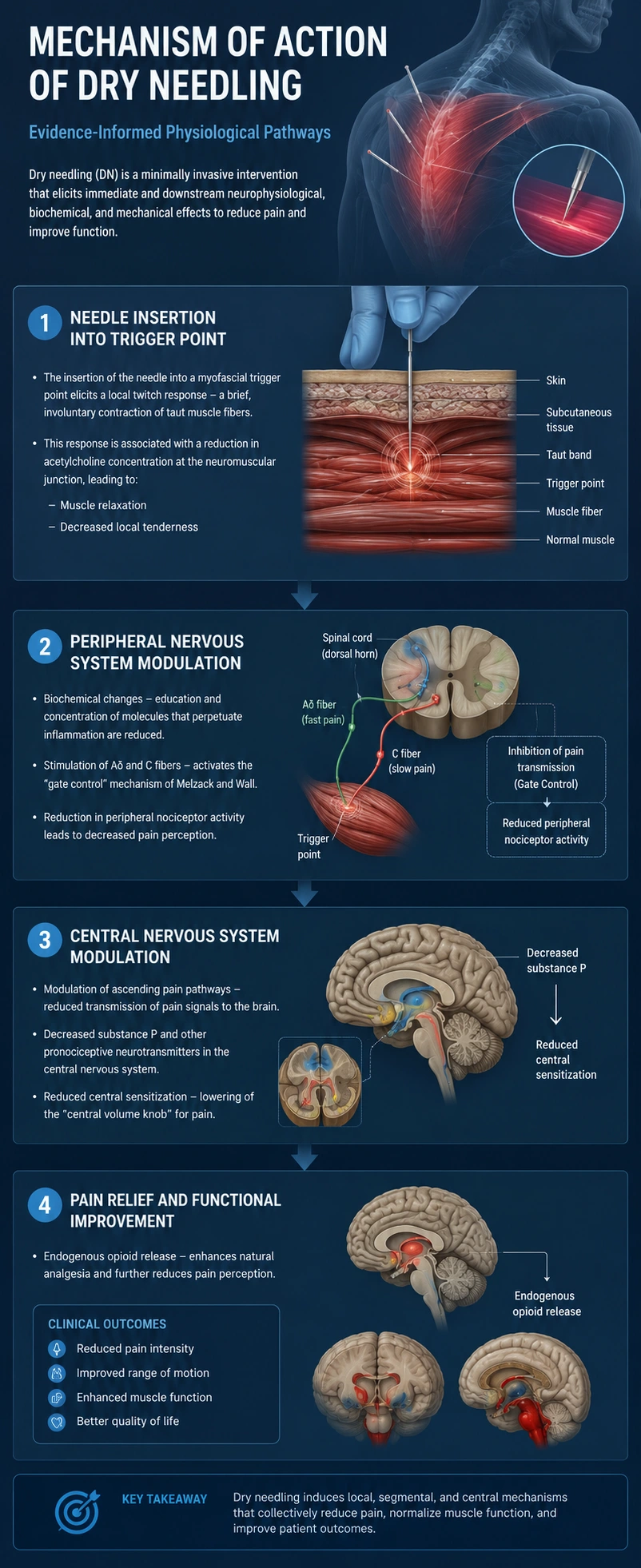
Mechanism of Action of Dry Needling
The therapeutic effect of dry needling begins with the insertion of a fine, sterile needle into a myofascial trigger point. This mechanical stimulation leads to the neutralization of the trigger point, resulting in muscle relaxation, pain reduction, and increased local blood flow. Improved circulation enhances oxygen delivery and removal of metabolic waste, which helps restore normal muscle function and expand the range of motion.
At the peripheral level, needle insertion reduces the release of inflammatory mediators from nerve endings within the tissue. This biochemical modulation decreases local inflammation and contributes to lower peripheral pain sensitivity. Simultaneously, activation of sensory fibers (Aδ and C fibers) engages the gate‑control mechanism, further dampening pain transmission.
Within the spinal cord, dry needling influences neurons in the dorsal horn, leading to inhibition of pain signal transmission toward the brain. A reduction in Substance P levels helps limit central sensitization, which is particularly beneficial in chronic pain conditions.
At the supraspinal level, stimulation of afferent pathways promotes the release of endogenous opioids such as endorphins and enkephalins in the brainstem. These natural pain‑modulating substances enhance descending inhibitory control, providing a systemic analgesic effect.
Summary
Dry needling acts through multilevel mechanisms — local muscular, peripheral, spinal, and central — to reduce pain, normalize muscle tone, and improve functional movement.
Clinical Indications — Conditions Treatable with Dry Needling
In broad terms, dry needling can be applied to any condition in which pain originates primarily or partially from muscles and their fascial coverings. By targeting myofascial trigger points and dysfunctional muscle fibers, the technique helps reduce pain, restore normal muscle tone, and improve movement patterns. Beyond muscular sources of pain, dry needling has also shown effectiveness in conditions involving tendons, joints, and peripheral nerves.
Chronic Pain Syndromes
Dry needling has demonstrated efficacy in managing fibromyalgia, chronic low back pain, chronic neck pain, and tension‑type headaches. By modulating peripheral and central pain pathways, it can reduce pain intensity and improve daily function.
Myofascial Pain and Muscle Tension
Conditions such as myofascial pain syndrome, muscle strain, and overuse syndromes often involve localized trigger points. Targeted needling of these points helps relieve pain, decrease muscle tightness, and restore normal contractile function.
Sports Injuries
Athletes frequently use dry needling to accelerate recovery from muscle strains, tendinopathies, and overuse injuries. The technique promotes local circulation, reduces pain, and supports optimal performance during rehabilitation.
Postural Disorders
Poor posture can lead to muscular imbalance and discomfort. Dry needling assists in releasing tension within postural muscles, facilitating postural correction and reducing compensatory pain patterns.
Restricted Range of Motion
Muscle tightness, scar tissue, or chronic inflammation can limit joint mobility. Dry needling improves muscle extensibility and joint range of motion, often complementing stretching and manual therapy.
Movement Disorders and Spasticity
In selected cases, dry needling may help reduce muscle hyperactivity and spasticity in patients with neurological conditions such as dystonia or post‑stroke spasticity, improving functional movement and comfort.
Migraine and Headache Disorders
Dry needling can reduce the frequency and severity of migraine attacks by addressing trigger points in cervical and cranial muscles that contribute to referred pain and tension.
Tendinopathies
In conditions such as Achilles tendinopathy, patellar tendinopathy, or lateral epicondylitis, dry needling stimulates local healing responses, enhances collagen remodeling, and alleviates pain.
Osteoarthritis
Dry needling may help relieve joint pain and stiffness associated with osteoarthritis by reducing periarticular muscle tension and improving local circulation.
Peripheral Neuropathies
Certain neuropathic conditions, such as carpal tunnel syndrome, can benefit from dry needling through pain modulation, muscle relaxation, and improved nerve mobility.
Effectiveness of Dry Needling in Musculoskeletal Conditions
Scientific evidence shows that dry needling can provide short‑term pain reduction and symptomatic relief across a range of musculoskeletal disorders. The strongest effects are consistently observed in conditions involving myofascial trigger points, although benefits have also been reported in tendinopathies and chronic pain syndromes.
Short‑Term Pain Reduction
A systematic review of randomized controlled trials found that dry needling produced statistically significant short‑term improvements in pain in conditions affecting the lower quarter (knee, thigh, low back, plantar region). However, these effects were not maintained at long‑term follow‑up, and no consistent improvements were observed in range of motion, strength, or quality of life 1.
Effectiveness in Tendinopathies
A network meta‑analysis evaluating treatments for tendinopathies (including rotator cuff, patellar, and Achilles tendinopathy) reported that dry needling produced pain improvements comparable to corticosteroid, saline, and local anesthetic injections, with no significant differences between these control interventions. This suggests that dry needling may be a reasonable conservative option for managing tendon‑related pain 1.
Myofascial Pain Syndromes
Across multiple systematic reviews, dry needling consistently demonstrates benefit in reducing pain associated with myofascial trigger points, particularly in the neck, shoulder, and lumbar regions. These improvements are attributed to neuromuscular modulation and biochemical changes at the trigger point level 1.
Chronic Pain Conditions
Evidence indicates that dry needling can reduce pain intensity in chronic musculoskeletal conditions such as chronic low back pain and chronic neck pain, although functional improvements are less consistent. The analgesic effect appears strongest in the acute and subacute phases following treatment.
Limitations of Current Evidence
A major review of 15 systematic reviews and meta‑analyses concluded that although dry needling is increasingly used, evidence quality is variable, and many studies have methodological limitations, including small sample sizes and short follow‑up periods. More high‑quality research is needed to determine long‑term effectiveness and optimal treatment protocols 2.
Summary
Overall, current scientific evidence supports dry needling as an effective short‑term intervention for reducing pain in a variety of musculoskeletal conditions, particularly those involving myofascial trigger points. Its role in improving long‑term outcomes, functional capacity, and quality of life remains less clear and requires further research.
Dry Needling vs. Acupuncture
Although dry needling and acupuncture both use thin, solid filiform needles, they are fundamentally different therapeutic approaches with distinct theoretical foundations, clinical goals, and mechanisms of action. Understanding these differences is essential for patients and clinicians when choosing the most appropriate intervention.
1. Theoretical Foundations
- Dry Needling is based on Western medical science, particularly anatomy, neurophysiology, and the concept of myofascial trigger points. The primary goal is to deactivate dysfunctional muscle tissue, reduce pain, and restore normal movement.
- Acupuncture originates from Traditional Chinese Medicine (TCM) and is grounded in the concept of meridians and the flow of vital energy (qi). Treatment aims to restore energetic balance and support systemic health.
2. Treatment Targets
- Dry Needling targets trigger points, taut muscle bands, dysfunctional motor endplates, and specific neuromuscular structures.
- Acupuncture targets acupuncture points located along meridians, which may or may not correspond to muscular or anatomical structures.
3. Mechanism of Action
- Dry Needling works through:
- mechanical disruption of trigger points
- modulation of peripheral and central pain pathways
- improved local blood flow
- reduction of inflammatory mediators
- activation of endogenous opioid systems
- Acupuncture is believed to work through:
- modulation of qi flow
- neurohumoral responses
- autonomic regulation
- systemic homeostatic effects
Although both techniques can influence the nervous system, dry needling’s mechanisms are specifically tied to musculoskeletal dysfunction, while acupuncture’s effects are broader and rooted in TCM principles.
4. Clinical Goals
- Dry Needling aims to:
- reduce myofascial pain
- normalize muscle tone
- improve range of motion
- restore functional movement
- Acupuncture aims to:
- balance energy flow
- support general wellness
- address systemic symptoms (e.g., sleep, digestion, stress)
5. Practitioner Training
- Dry Needling is performed by clinicians trained in anatomy, musculoskeletal medicine, and trigger point therapy (physiatrists, physical therapists, sports medicine clinicians).
- Acupuncture is performed by practitioners trained in Traditional Chinese Medicine, often with multi‑year specialized education.
6. Overlap and Misconceptions
While both techniques use similar needles, they are not interchangeable. Dry needling is not a form of acupuncture, and acupuncture is not a trigger‑point therapy
What to Expect During a Dry Needling Treatment
Before beginning a dry needling treatment, the clinician explains the procedure, expected effects, and possible side effects to ensure the patient feels informed and comfortable. The treatment room should be warm and calm, and most patients are positioned lying down to maximize comfort and prevent unnecessary muscle tension. The area being treated is exposed, and the only instrument used is a sterile, single‑use filiform needle.
Although the needle resembles an acupuncture needle, it is extremely thin — roughly 2.5 times the thickness of a human hair. Using a plastic guide tube, the clinician taps the needle through the skin with a quick, gentle motion to minimize discomfort. The needle is then advanced slowly and precisely into the target tissue. Once inserted, the needle typically remains in place for 5–15 minutes, during which the clinician may adjust its depth or angle to further stimulate the tissue and enhance the therapeutic effect. It is important for the patient to remain still while the needles are in place.
During the dry needling treatment, patients may feel a brief, sharp sensation or a local twitch response, which is a normal and often desirable reaction indicating that the trigger point has been activated. Mild pressure, heaviness, or a dull ache around the needle site is also common. Throughout the session, the patient maintains communication with the clinician to ensure comfort and safety. At the end of the treatment, all needles are removed and disposed of in approved medical sharps containers.
Aftercare Advice Following a Dry Needling Treatment
After completing a dry needling treatment, proper aftercare helps support tissue recovery, reduce post‑treatment discomfort, and enhance the overall therapeutic effect. Although dry needling is a minimally invasive procedure, the body still undergoes a localized healing response, so thoughtful post‑treatment habits can make a meaningful difference.
Stay Well Hydrated
Drinking enough water after a dry needling treatment supports circulation, tissue recovery, and the natural clearance of metabolic by‑products released during trigger‑point stimulation. Hydration also helps reduce the likelihood of post‑treatment soreness.
Avoid Strenuous Physical Activity
Even though the procedure is minimally invasive, the treated muscles may be temporarily sensitive. It is helpful to avoid heavy lifting, high‑intensity exercise, or repetitive strain for the next 24–48 hours. Gentle movement, walking, and light stretching are generally well tolerated and can support recovery.
Expect Mild Soreness
Some patients experience a sensation similar to post‑exercise muscle soreness. This is normal and typically resolves within a day or two. Gentle heat, light mobility exercises, and hydration can help ease discomfort.
Listen to Your Body
Fatigue, mild heaviness, or temporary stiffness can occur after a dry needling treatment. These sensations usually improve quickly. If anything feels unusual or persists longer than expected, it is important to contact a qualified healthcare professional for guidance.
Support the Healing Process
Healthy habits such as adequate sleep, balanced nutrition, and avoiding alcohol immediately after treatment can help the body respond optimally to the intervention.
Safety and Side Effects of Dry Needling
Dry needling is considered a very safe treatment method when performed by a trained and licensed healthcare professional. Complications are rare, and most side effects—if they occur—are mild and short‑lived. Understanding what is normal and what is uncommon helps patients feel more confident and informed before undergoing a dry needling treatment.
Overall Safety Profile
Dry needling is a minimally invasive technique that uses sterile, single‑use filiform needles. In experienced hands, the procedure carries no significant risks for the vast majority of patients. Most reactions are mild, temporary, and part of the normal physiological response to tissue stimulation.
Common and Mild Side Effects
These effects are generally harmless and resolve within hours to a couple of days:
- Mild bleeding at the needle site after removal
- Small bruises, often due to increased local blood flow
- Temporary soreness similar to post‑exercise muscle discomfort
- Local warmth or heaviness in the treated area
These reactions reflect increased circulation and tissue activation, which are part of the therapeutic process.
Autonomic Nervous System Reactions
A small number of patients—especially those with heightened autonomic sensitivity—may experience transient systemic reactions such as:
- lightheadedness or brief dizziness
- sweating or a sudden feeling of heat
- changes in blood pressure
- palpitations or a sensation of rapid heartbeat
- shortness of breath
These reactions are rare, usually short‑lasting, and resolve quickly with rest. Maintaining communication with the clinician during the session helps ensure comfort and safety.
Rare Side Effects
Although extremely uncommon, the following complications may occur, typically only in cases of improper technique or inadequate anatomical knowledge:
- Infection at the needle site (prevented by using sterile, single‑use needles)
- Pneumothorax, a very rare complication when needling near the thoracic region without proper expertise
- Nerve or blood vessel puncture, also very rare and associated with incorrect technique
- Needle breakage, exceptionally rare with modern high‑quality needles
When dry needling is performed by a qualified clinician with appropriate anatomical training, these risks are extraordinarily low.
Summary
Dry needling dry needling is a safe, evidence‑informed, and well‑tolerated therapeutic method. Most side effects are mild and temporary, while serious complications are exceedingly rare when the procedure is performed by trained professionals. Proper patient education, sterile technique, and anatomical precision are key factors that ensure a safe and effective treatment experience.
Frequently Asked Questions About Dry Needling
This section addresses the most common questions patients have before starting a dry needling treatment, helping them feel informed, safe, and confident.
1. What is dry needling and how does it work?
Dry needling is a therapeutic technique in which a clinician inserts thin, sterile filiform needles into specific points within the muscle to reduce pain, release tension, and improve function. The needle is called “dry” because no medication or fluid is injected. Its effect comes from mechanical stimulation of trigger points and modulation of the nervous system.
2. Does dry needling hurt?
Most patients describe the sensation as mild and brief discomfort, often followed by a feeling of release. A short muscle twitch may occur when the needle reaches a trigger point — this is normal and often desirable. After the session, temporary soreness or heaviness may appear but usually resolves quickly.
3. How many treatments will I need?
The number of sessions depends on the condition being treated, its severity, and individual response. Some patients feel improvement after 1–3 sessions, while others require a longer treatment plan. Your clinician will provide personalized recommendations.
4. Who is qualified to perform dry needling?
Dry needling should be performed only by trained and licensed healthcare professionals, such as physiatrists, physicians, or specially trained physical therapists with formal education in anatomy and dry needling techniques.
5. Is dry needling suitable for everyone?
Not always. Certain medical conditions, medications, or pregnancy may require caution or represent contraindications. A qualified clinician will assess your medical history to determine whether dry needling is appropriate for you.
6. How should I prepare for a dry needling treatment?
Inform your clinician about your medical history, allergies, and medications. Wear comfortable clothing that allows access to the treatment area, and make sure you are well hydrated before the session.
Conclusion
Dry needling is a highly individualized therapeutic technique that allows clinicians to tailor treatment to each patient’s unique needs, anatomy, and functional goals. It has proven to be an effective and safe method for a wide range of musculoskeletal conditions, including chronic pain syndromes, sports injuries, muscle tension, postural dysfunctions, and various movement‑related disorders.
Dommerholt J, Chou LW, Finnegan M, Hooks T. A Critical Overview of the Current Myofascial Pain Literature. Journal of Bodywork and Movement Therapies. 2018;22(2):402-410. Review: Comprehensive overview of myofascial pain mechanisms and trigger point management
Dommerholt J. Trigger Point Dry Needling. Journal of Manual & Manipulative Therapy. 2006;14(4):70E-87E. Clinical overview: Mechanisms, indications, and application principles of trigger point dry needling
Kietrys DM, et al. Effectiveness of Dry Needling for Upper-Quarter Myofascial Pain. Journal of Orthopaedic & Sports Physical Therapy. Systematic review: Dry needling reduces pain in neck and shoulder myofascial pain syndromes
Gattie E, et al. The Effectiveness of Trigger Point Dry Needling for Musculoskeletal Conditions. Journal of Manual & Manipulative Therapy. Meta-analysis: Short-term pain reduction across multiple musculoskeletal conditions
Hernández-Secorún M, Abenia-Benedí H, Borrella-Andrés S, Marqués-García I, Lucha-López MO, Herrero P, Iguacel I, Tricás-Moreno JM, Hidalgo-García C. Effectiveness of Dry Needling in Improving Pain and Function in Comparison with Other Techniques in Patients with Chronic Neck Pain. Pain Research and Management. 2023. Systematic review and meta-analysis: Dry needling improves pain and function in chronic neck pain
Rodríguez-Huguet M, Vinolo-Gil MJ, Góngora-Rodríguez J. Dry Needling in Physical Therapy Treatment of Chronic Neck Pain. Journal of Clinical Medicine. 2022;11(9):2370. Systematic review: Evidence supports dry needling as part of chronic neck pain rehabilitation