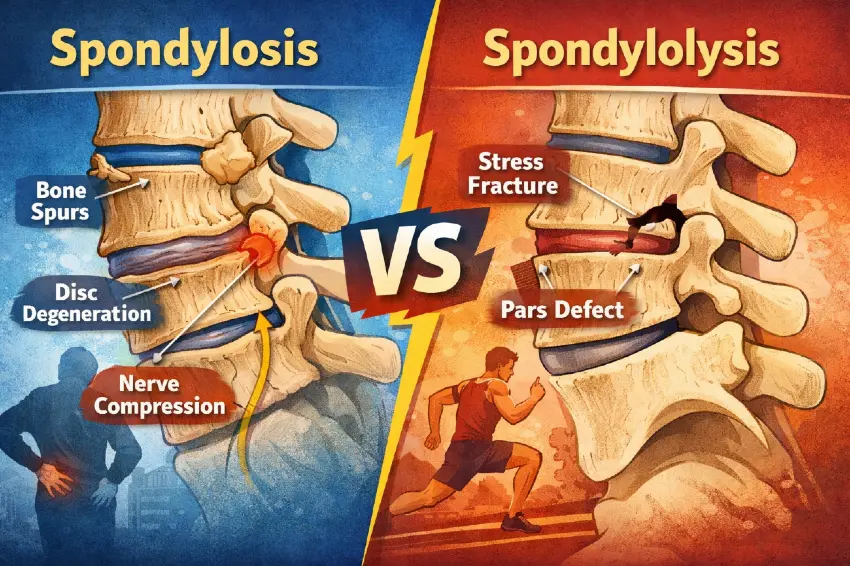
Spondylosis and spondylolysis are two distinct spinal conditions that are often confused, yet they differ significantly in their causes, structure, and clinical impact. While spondylosis is a degenerative condition associated with aging and long-term wear and tear, spondylolysis is a structural defect or stress fracture that typically affects younger, more active individuals.
As a physician specializing in physical medicine and rehabilitation, I frequently see patients who are unsure whether their back pain is due to degenerative changes or a structural defect in the spine.
Understanding these key differences is essential for accurate diagnosis, appropriate treatment planning, and long-term spinal health. The comparison below highlights the most important distinctions between these two conditions at a glance.
Spondylosis vs Spondylolysis: Key Differences at a Glance
| Feature | Spondylosis | Spondylolysis |
|---|---|---|
| Type of condition | Degenerative spine condition caused by aging and wear and tear | Structural defect or stress fracture in the pars interarticularis |
| Primary cause | Age-related degeneration, disc dehydration, and joint wear | Repetitive stress, overuse, or mechanical trauma |
| Spinal structure affected | Intervertebral discs, facet joints, and vertebrae | Pars interarticularis (small part of the vertebra) |
| Spinal stability | Generally stable, with gradual stiffness and reduced mobility | May cause instability and can progress to vertebral slippage |
| Typical symptoms | Chronic back or neck pain, stiffness, reduced range of motion | Activity-related lower back pain, especially with extension |
| Pain pattern | Constant or chronic pain that worsens with age | Pain triggered by physical activity and relieved by rest |
| Typical age group | Older adults (age-related condition) | Young athletes and active individuals |
| Risk of progression | Slow progression, usually chronic but stable | Can progress to spondylolisthesis if untreated |
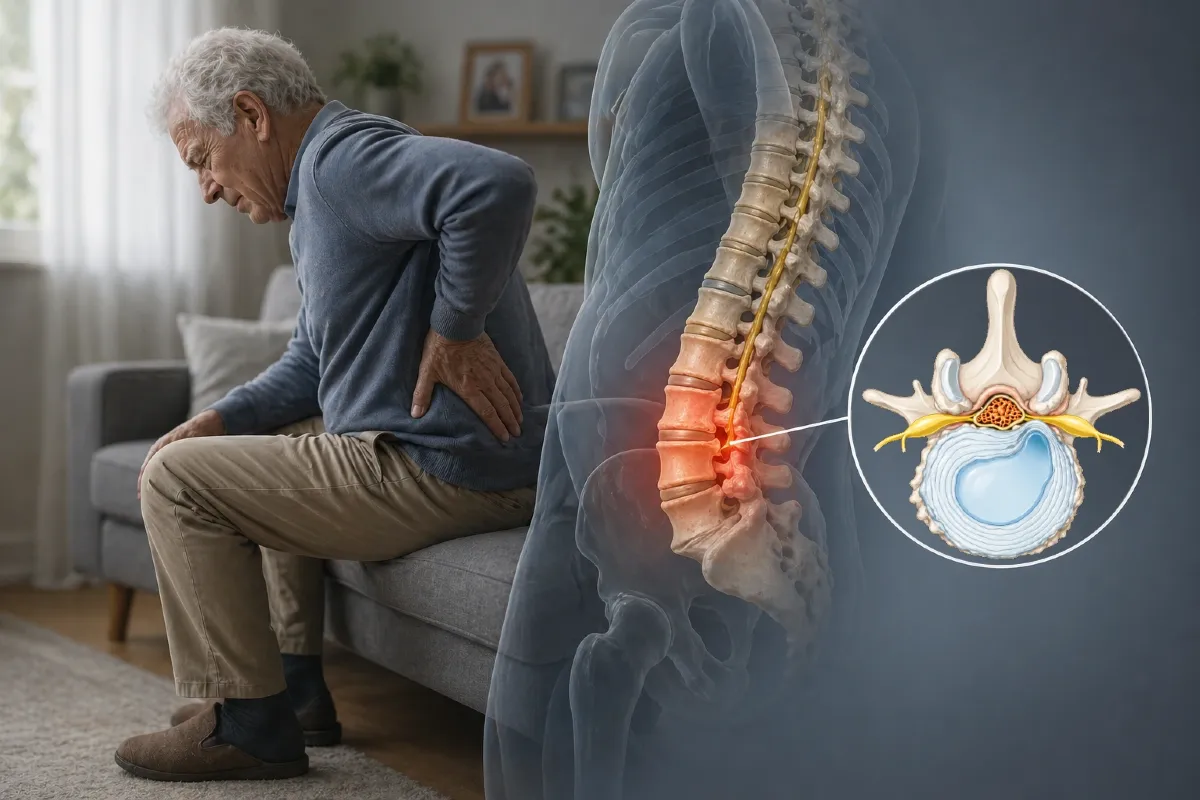
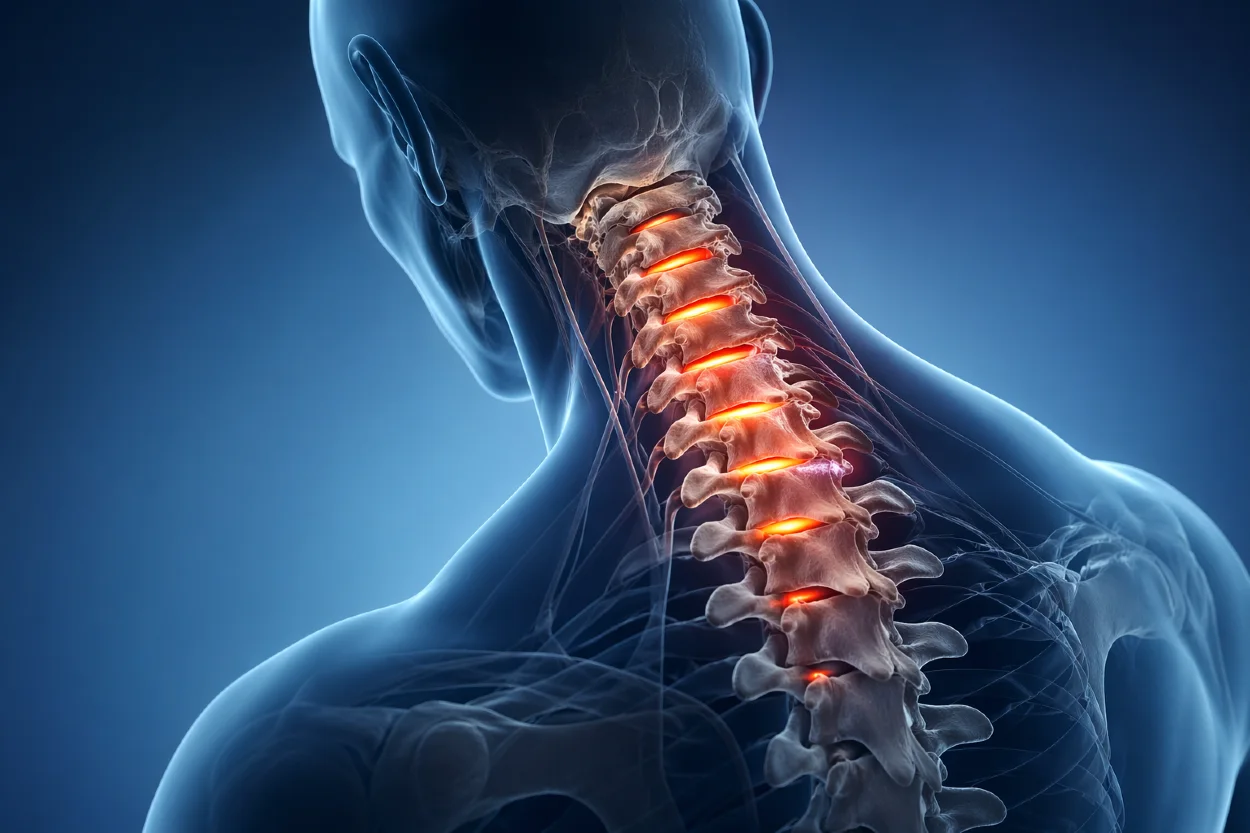
What Is Spondylosis?
Spondylosis is a degenerative condition of the spine associated with aging and cumulative mechanical stress.
It affects multiple spinal structures, including:
- intervertebral discs
- facet joints
- vertebral bodies
Over time, the spine undergoes:
- disc dehydration and height loss
- formation of osteophytes (bone spurs)
- joint degeneration
These changes may contribute to chronic back pain, stiffness, and reduced mobility.
👉 Spondylosis is commonly referred to as spinal osteoarthritis.
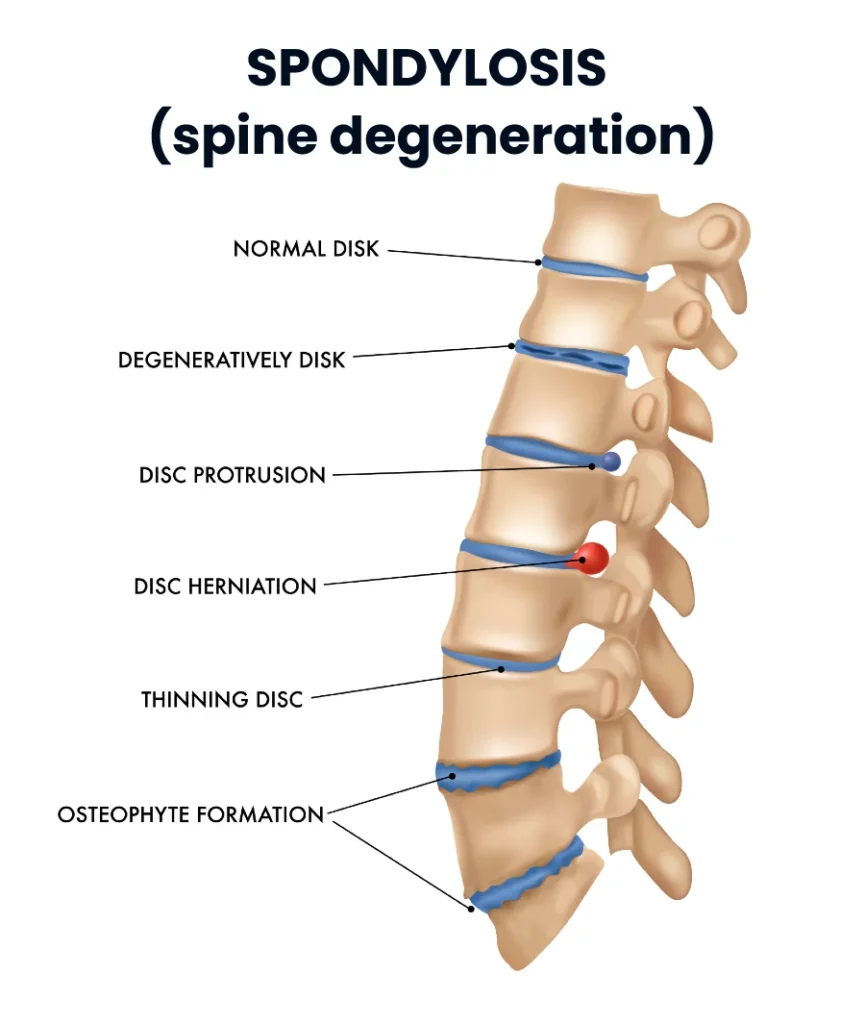
To learn more about this condition, read our detailed guide on spondylosis here: Spondylosis: What It Really Is, Risk Factors, Symptoms, and Treatment
What Is Spondylolysis?
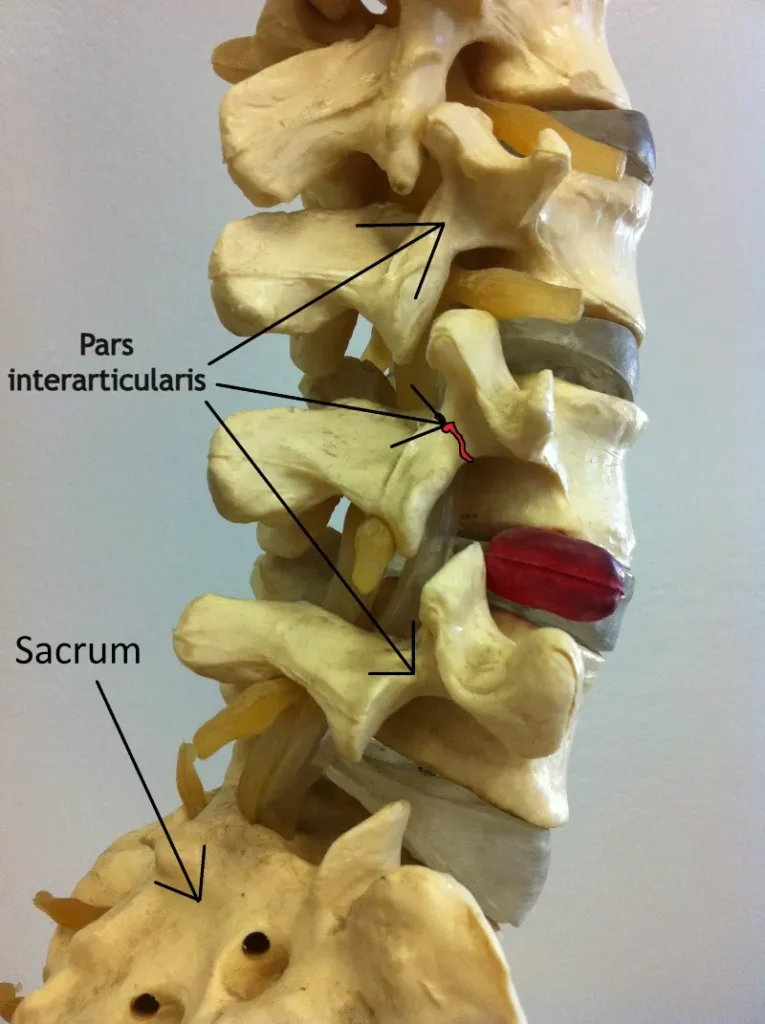
Spondylolysis is a defect or stress fracture in the pars interarticularis, a small segment of the vertebra.
This condition is most often:
- located at L5
- caused by repetitive spinal extension
- seen in young athletes
Unlike spondylosis, spondylolysis is not primarily degenerative but rather a mechanical injury to bone.
If left untreated, it can progress and, in some cases, lead to spondylolisthesis (vertebral slippage).
For a more in-depth explanation of causes, symptoms, and treatment options, visit our full article on spondylolisis:
👉 Spondylolysis: The Most Common Cause of Lower Back Pain in Young Athletes
Spondylosis vs Spondylolysis: Key Differences
Spondylosis vs spondylolysis are two different spinal conditions. Spondylosis is a degenerative condition caused by age-related wear and tear of the spine, while spondylolysis is a structural defect or stress fracture in a vertebra. The main difference is that spondylosis affects spinal discs and joints over time, whereas spondylolysis involves a specific fracture that can impact spinal stability and is often seen in younger, active individuals.
Structure of the Problem
The key difference lies in how each condition affects the spine.
Spondylosis involves gradual degeneration of spinal components over time, leading to disc height loss, joint wear, and reduced mobility, but typically without vertebral displacement.
Spondylolysis involves a defect in the vertebra, specifically in the pars interarticularis, which may compromise structural integrity and spinal alignment.
This distinction is crucial when evaluating spinal imaging and planning treatment, as it directly influences diagnosis and management decisions.
Underlying Mechanism
Spondylosis Mechanism
Spondylosis develops as a result of age-related changes in the spine, including:
- aging-related disc degeneration
- loss of hydration in intervertebral discs
- increased load on facet joints
- formation of osteophytes
These changes are part of the natural aging process but can be accelerated by poor posture, repetitive strain, and a sedentary lifestyle.
Spondylolysis Mechanism
Spondylolysis results from repetitive stress and mechanical overload on the spine, leading to stress fractures in the pars interarticularis. This condition is especially common in activities involving:
- hyperextension
- rotation
- repetitive impact
It is frequently observed in sports such as gymnastics, football, and weightlifting, where repetitive spinal loading increases the risk of injury.
Spinal Stability
Spinal stability is one of the most important distinctions in spondylosis vs spondylolysis.
Spondylosis may cause stiffness and reduced mobility but generally preserves spinal alignment.
Spondylolysis may lead to structural weakness and instability, particularly if the defect is bilateral.
This difference in stability is clinically important, as it influences treatment decisions, activity restrictions, and the risk of progression. In some cases, spondylolysis may progress to spondylolisthesis, where one vertebra slips forward.
Symptoms Comparison
Spondylosis Symptoms
- Chronic neck or lower back pain
- Morning stiffness
- Reduced flexibility
- Occasional nerve compression symptoms
Spondylolysis Symptoms
- Pain localized to the lower back
- Pain worsened by activity or extension
- Relief with rest
- Possible muscle tightness
- Reduced performance in sports
While both conditions can cause back pain, the underlying pattern of symptoms often helps distinguish between degenerative and structural causes. Spondylolysis is more likely to present with activity-related pain, while spondylosis is often chronic and progressive.
Who Is More Affected?
Spondylosis
- Primarily affects older adults
- Strongly associated with aging
- Common in individuals over 50
Spondylolysis
- Common in young athletes
- Seen in adolescents and young adults
- Associated with repetitive spinal stress
This age-related difference is one of the key clinical clues used to differentiate between spondylosis and spondylolysis during diagnosis. It also helps guide imaging decisions and treatment planning.
Diagnosis and Imaging
Diagnosis of spondylosis vs spondylolysis is based on a combination of clinical examination and imaging studies. Because these conditions have different causes—degenerative changes vs structural defect—the correct diagnosis is essential for effective treatment.
Clinical Examination
- Spondylosis: chronic pain, stiffness, reduced mobility
- Spondylolysis: pain with extension, improves with rest, activity-related symptoms
👉 Clinical tests can help identify pain patterns, especially in spondylolysis.
Imaging (X-ray, MRI, CT)
X-ray
- Shows disc degeneration and osteophytes in spondylosis
- May show pars defects in spondylolysis (not always early)
MRI
- Detects soft tissue changes and nerve compression
- Shows early stress reactions in spondylolysis
CT Scan
- Best for detecting pars interarticularis fracture
- Most accurate for confirming spondylolysis
Key Difference on Imaging
- Spondylosis → degenerative changes, no fracture
- Spondylolysis → visible defect (stress fracture) in vertebra
Treatment
Treatment of spondylosis vs spondylolysis depends on the severity of symptoms, the degree of structural change, and how much the condition affects daily function. In most cases, conservative treatment is the first-line approach, while surgery is reserved for more severe or persistent cases.
Conservative Treatment
Spondylosis Treatment
Management of spondylosis focuses on reducing pain, improving mobility, and slowing progression of degenerative changes:
- Physical therapy to improve posture, strength, and spinal stability
- Exercise programs targeting core and paraspinal muscles
- Pain management (e.g., NSAIDs, short-term analgesics)
- Lifestyle modification such as weight control and ergonomic adjustments
- Manual therapy in selected cases
👉 The goal is to manage chronic degenerative pain and maintain function.
Spondylolysis Treatment
Treatment of spondylolysis focuses on allowing the stress fracture to heal:
- Rest and activity modification, especially avoiding extension and rotation
- Temporary bracing in some cases
- Physical therapy after the acute phase
- Gradual return to activity under supervision
👉 In young athletes, early diagnosis and proper management are crucial to prevent progression to spondylolisthesis.
When Is Surgery Needed?
Surgery is not required in most cases, but may be considered when:
- Severe or persistent pain does not improve with conservative treatment
- There is progressive neurological deficit (e.g., weakness, numbness)
- In spondylolysis, there is non-healing fracture or progression to spondylolisthesis
- Significant spinal instability is present
Common surgical options include:
- Spinal fusion
- Decompression procedures (when nerve compression is involved)
Clinical Insight
In clinical practice, the majority of patients with both spondylosis and spondylolysis respond well to non-surgical treatment. Early recognition and accurate diagnosis are essential for guiding effective management.
A structured rehabilitation program, tailored to the patient’s condition and activity level, plays a key role in reducing symptoms and improving long-term outcomes.
Surgery remains the exception rather than the rule and is typically reserved for refractory or more complex cases where conservative treatment is not sufficient.
When to Seek Medical Help
Understanding when to seek medical attention for spondylosis vs spondylolysis is essential for preventing complications and ensuring timely treatment. While both conditions can often be managed conservatively, certain symptoms—known as red flags—require prompt medical evaluation.
Red Flag Symptoms
You should seek medical help if you experience any of the following:
- Severe or worsening pain that does not improve with rest or medication
- Radiating pain into the arms or legs, which may indicate nerve compression
- Numbness, tingling, or weakness in the limbs
- Loss of coordination or difficulty walking
- Bowel or bladder dysfunction (a potential sign of serious nerve involvement)
- Progressive pain with neurological symptoms
- Pain following trauma or injury, especially if sudden and intense
👉 In the context of spondylolysis, worsening symptoms may indicate progression toward spondylolisthesis, where vertebral slippage increases the risk of spinal instability and nerve compression.
When Symptoms Should Not Be Ignored
While mild back pain is common in both conditions, it should not be ignored if:
- It persists for more than a few weeks
- It interferes with daily activities or sleep
- It becomes progressively worse over time
- It is associated with neurological symptoms
👉 Early evaluation allows for timely diagnosis, appropriate imaging, and the prevention of further spinal damage.
Clinical Insight
In clinical practice, many patients delay seeking care until symptoms significantly worsen. However, early diagnosis and intervention are key to preventing complications in both spondylosis and spondylolysis.
As a general rule, any new neurological symptoms, rapidly worsening pain, or functional impairment should be assessed by a healthcare professional without delay.
Frequently Asked Questions (FAQ)
Is spondylosis the same as spondylolysis?
No, spondylosis vs spondylolysis are two different spinal conditions. Spondylosis is a degenerative condition caused by aging and wear and tear, affecting the discs and joints over time. In contrast, spondylolysis is a structural defect or stress fracture in the vertebra, most often in the pars interarticularis. Although they can cause similar symptoms, their underlying causes and treatment approaches are different.
Which condition is more serious?
Neither condition is always more serious—it depends on the severity of symptoms and progression. Spondylosis is usually a slow, degenerative process and may remain mild for many years. Spondylolysis, however, can become more serious if it leads to instability or progresses to spondylolisthesis, especially if left untreated. Severe cases of either condition may require medical intervention.
Can you have both at the same time?
Yes, it is possible to have both spondylosis and spondylolysis simultaneously. In some cases, degenerative changes from spondylosis may weaken spinal structures and contribute to the development of a stress fracture seen in spondylolysis. This overlap is more common in older adults, but it can occur in different age groups depending on risk factors.
Is spondylolysis always painful?
No, spondylolysis is not always painful. Some individuals may have the condition without any noticeable symptoms, especially in early or mild cases. However, when symptoms are present, they often include lower back pain, particularly during activity or spinal extension, and may improve with rest. Pain can vary depending on the severity of the defect and associated inflammation.
Conclusion
Understanding spondylosis vs spondylolysis is essential for accurate diagnosis, effective treatment, and long-term spinal health. Although both conditions affect the spine, spondylosis is a degenerative condition, while spondylolysis is a structural defect that may lead to instability.
Early recognition of symptoms, proper imaging, and a tailored treatment approach can significantly improve outcomes and reduce the risk of complications. Most patients respond well to conservative management, including physical therapy and lifestyle modification, while surgery is reserved for more severe or refractory cases.
If you are experiencing persistent back or neck pain, especially with neurological symptoms, seeking medical evaluation is crucial for timely diagnosis and appropriate care.
StatPearls Publishing. Lumbar Spondylolysis and Spondylolisthesis. Treasure Island (FL): StatPearls; 2025.
Binder AI. Cervical Spondylosis. StatPearls Publishing; 2025.
Kalichman L, Hunter DJ. Spondylolysis and spondylolisthesis: prevalence and association with low back pain. Spine (Phila Pa 1976). 2009;34(2):199–205.
Standaert CJ, Herring SA. Spondylolysis: a critical review. Br J Sports Med. 2005;39(7):415–422.
Genevay S, Atlas SJ. Lumbar spinal stenosis. Best Pract Res Clin Rheumatol. 2010;24(2):253–265.
Modic MT, Ross JS. Lumbar degenerative disk disease. Radiology. 2007;245(1):43–61.
Campbell RS, Grainger AJ. Imaging of spondylolysis. Clin Radiol. 2003;58(6):411–419.
American Academy of Orthopaedic Surgeons. Spondylolysis and Spondylolisthesis.
Cleveland Clinic. Spondylosis (Spinal Osteoarthritis).
Cleveland Clinic. Spondylolysis.