Total hip arthroplasty (THA), commonly referred to as total hip replacement, is one of the most frequently performed and successful orthopedic procedures in the United States. This surgical intervention is designed to relieve chronic hip pain, restore mobility, and significantly improve quality of life for patients suffering from advanced joint damage.
With an aging population and rising rates of degenerative joint conditions such as osteoarthritis, the demand for total hip arthroplasty continues to grow across the U.S. THA is typically recommended when conservative treatments—such as physical therapy, medications, or lifestyle modifications—no longer provide sufficient relief.
In this article, we’ll cover everything you need to know about total hip arthroplasty (THA), including when it’s needed, how the procedure works, recovery expectations, and long-term outcomes.
Key Clinical Points – Total Hip Arthroplasty (THA)
- Total hip arthroplasty (THA) is a highly effective procedure that replaces a damaged hip joint to relieve pain and restore mobility.
- The most common indication is end-stage osteoarthritis, but THA is also performed for avascular necrosis, rheumatoid arthritis, and hip fractures.
- Patient selection is based on persistent pain, reduced function, and failure of conservative treatments such as physiotherapy and injections.
- The procedure involves replacing the femoral head and acetabulum with prosthetic components that restore joint mechanics.
- Early mobilization and rehabilitation are essential for recovery and reducing complications such as thrombosis and stiffness.
- Most patients achieve significant pain relief, improved mobility, and long-term outcomes, with implants lasting 15–25 years or more.
What Is Total Hip Arthroplasty (THA)?
Total hip arthroplasty (THA), also known as total hip replacement, is a surgical procedure in which a damaged or diseased hip joint is replaced with an artificial implant. The main goal of THA is to relieve pain, restore joint function, and improve mobility and overall quality of life.
Overview of the Procedure
During the procedure, the surgeon removes the damaged bone and cartilage from both components of the hip joint: the femoral head (the ball) and the acetabulum (the socket in the pelvis). These structures are then replaced with prosthetic components designed to replicate natural hip movement.
THA vs Other Hip Procedures
Total hip arthroplasty differs from other hip procedures in terms of scope and indication:
- Total Hip Arthroplasty (THA): replaces both the femoral head and the acetabulum. It is indicated for advanced, end-stage joint disease.
- Hemiarthroplasty: replaces only the femoral head, most commonly used in selected hip fractures.
- Hip resurfacing: preserves more bone by capping the femoral head rather than fully replacing it. It is typically reserved for younger, more active patients.
Among these options, THA is considered the gold standard for treating severe degenerative hip conditions due to its ability to provide the most complete restoration of joint function.
Hip Implant (Prosthesis)
The artificial hip joint used in total hip arthroplasty consists of several key components:
- Acetabular component: a cup-shaped implant placed into the pelvic socket
- Femoral stem: inserted into the femur to provide stable fixation
- Femoral head: a ball component that replaces the natural femoral head
- Bearing surface: the interface between components that allows smooth movement with minimal friction
Modern hip implants are typically made from durable materials such as titanium alloys, ceramic, and highly cross-linked polyethylene, ensuring long-term durability and reduced wear.
When Is Total Hip Replacement Needed?
Total hip arthroplasty (THA), or total hip replacement, is performed to replace a damaged or worn-out hip joint with an artificial implant. This procedure is indicated in a variety of conditions that lead to progressive joint degeneration, persistent pain, and functional limitation.
The most common indication for hip replacement surgery is hip osteoarthritis. However, several other conditions can also lead to severe joint damage requiring THA. These include inflammatory arthritis, traumatic injuries, and structural abnormalities of the hip joint.
Below are the most common clinical indications for total hip arthroplasty:
Osteoarthritis (Hip Arthritis)
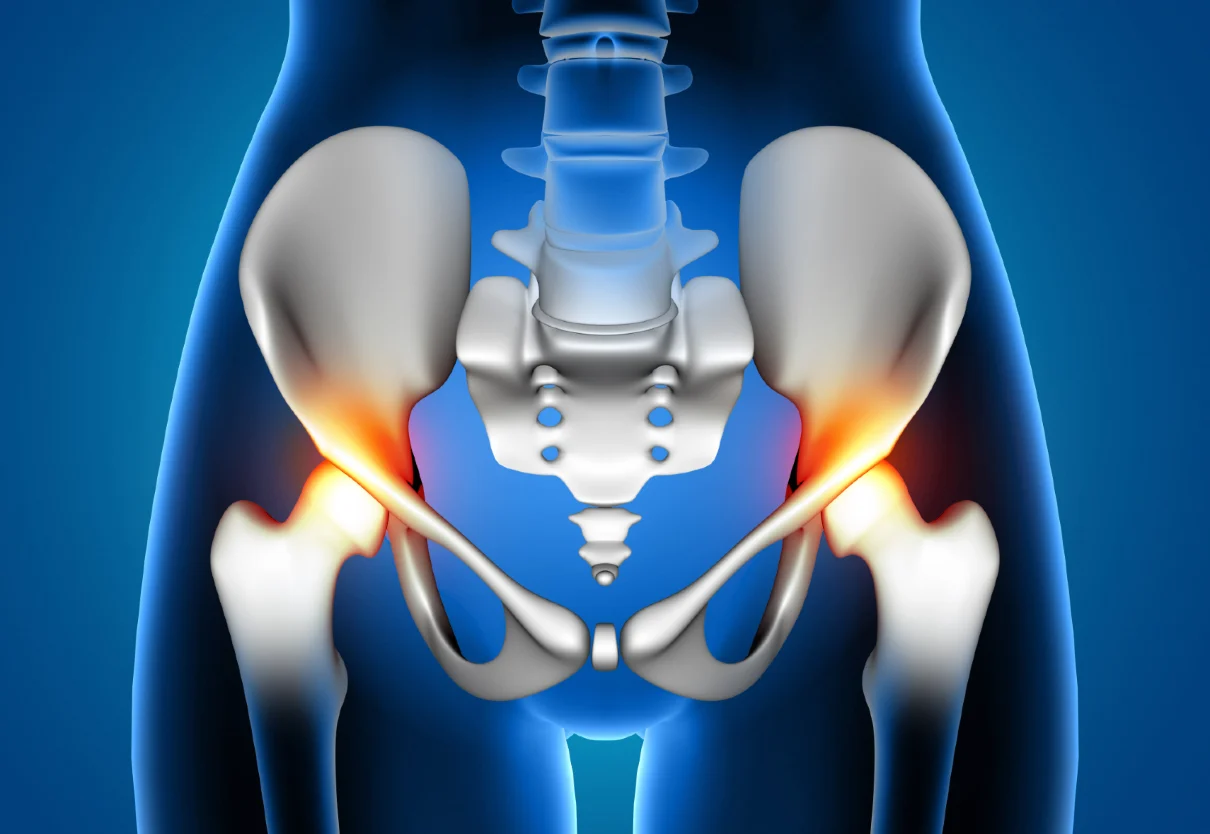
Osteoarthritis of the hip is the leading cause of total hip arthroplasty. It is a degenerative joint disease often referred to as “wear-and-tear arthritis.” It is characterized by the gradual breakdown of articular cartilage, narrowing of the joint space, formation of subchondral cysts, synovial inflammation, and the development of osteophytes (bone spurs).
Hip osteoarthritis most commonly affects individuals over the age of 50 and typically presents with:
- Groin or hip pain
- Stiffness, especially in the morning or after rest
- Progressive reduction in range of motion
Rheumatoid Arthritis
Rheumatoid arthritis is a chronic autoimmune inflammatory disease in which the synovial membrane becomes inflamed and thickened. Over time, this persistent inflammation can lead to cartilage destruction and severe joint damage.
Unlike osteoarthritis, rheumatoid arthritis is systemic and can affect multiple joints. In advanced stages, it may result in significant pain, stiffness, and functional disability, making total hip arthroplasty necessary.
Hip Fractures
Fractures of the femoral neck or proximal femur are a common indication for hip replacement, especially in older patients. These injuries usually occur after a fall or minor trauma and are often associated with osteoporosis.
In many cases, total hip arthroplasty is preferred when the fracture is displaced or when there is a high risk of poor healing or complications with other treatment options.
Post-Traumatic Arthritis
Post-traumatic arthritis develops after a previous injury to the hip joint, most commonly a fracture. Damage to the cartilage and surrounding structures leads to progressive degeneration, pain, stiffness, and inflammation over time.
Avascular (Aseptic) Necrosis of the Femoral Head
Avascular necrosis (AVN), also known as osteonecrosis, occurs when the blood supply to the femoral head is compromised, leading to bone cell death. This can result in structural collapse of the femoral head and severe joint destruction.
Common risk factors include trauma, long-term corticosteroid use, and excessive alcohol consumption.
Developmental Dysplasia of the Hip (DDH)
Developmental dysplasia of the hip is a congenital condition in which the hip joint does not develop properly. Depending on severity, this abnormal joint structure can lead to early cartilage wear and progressive joint degeneration.
Patients with significant dysplasia may require total hip arthroplasty at a younger age, sometimes in their 30s or 40s, due to accelerated joint deterioration.
Clinical Insight
Total hip arthroplasty is indicated when hip joint damage becomes severe enough to cause persistent pain, reduced mobility, and failure of conservative treatment options.
While osteoarthritis remains the most common indication, a wide range of degenerative, inflammatory, traumatic, and developmental conditions may ultimately lead to the need for hip replacement surgery.
Early recognition of the underlying pathology and timely referral for specialist evaluation are essential for optimizing functional outcomes and quality of life.
| Condition | Pathophysiology / Key Features | Clinical Relevance for THA |
|---|---|---|
| Osteoarthritis | Degenerative cartilage loss, joint space narrowing, osteophyte formation, subchondral cysts | Most common indication for total hip arthroplasty; progressive pain and stiffness refractory to conservative therapy |
| Rheumatoid Arthritis | Autoimmune synovial inflammation leading to cartilage destruction and joint erosion | Indication in advanced disease with severe pain, deformity, and functional limitation |
| Avascular Necrosis (AVN) | Disruption of blood supply to femoral head causing bone necrosis and potential collapse | Often requires THA once femoral head collapse and joint destruction occur |
| Hip Fracture | Fracture of femoral neck or proximal femur, often related to trauma and osteoporosis | THA indicated in displaced fractures or when poor healing prognosis is expected |
| Post-Traumatic Arthritis | Secondary degeneration following intra-articular injury with progressive cartilage damage | May require THA in chronic cases with persistent pain and loss of function |
| Developmental Dysplasia of the Hip (DDH) | Abnormal hip joint development leading to altered biomechanics and accelerated wear | Early-onset osteoarthritis; THA often required in younger patients |
What Does Total Hip Arthroplasty (THA) Involve?
Total hip arthroplasty (THA), also known as total hip replacement, is a surgical procedure in which the damaged parts of the hip joint are removed and replaced with artificial components (prosthesis). The goal of the operation is to relieve pain, restore function, and improve mobility.
Preoperative Preparation
Before surgery, patients undergo a detailed clinical assessment including physical examination, blood tests, and imaging (X-ray, sometimes CT or MRI). Medical optimization is important to reduce perioperative risks, including management of cardiovascular status, diabetes, and medications such as anticoagulants.
Preoperative planning also includes selecting the appropriate implant type and surgical approach based on anatomy, bone quality, and patient activity level.
Main Steps of the Procedure
The operation is typically performed under spinal or general anesthesia and involves the following key steps:
- The surgeon makes an incision to access the hip joint.
- The damaged femoral head (ball of the hip joint) is removed.
- The acetabulum (hip socket) is cleaned of damaged cartilage and reshaped.
- A metal acetabular cup is implanted into the socket, sometimes fixed with screws or bone cement.
- A liner made of polyethylene, ceramic, or metal is inserted into the cup to create a smooth bearing surface.
- The femoral canal is prepared, and a metal stem is inserted into the femur. This can be:
- Cemented fixation, where bone cement secures the implant
- Cementless fixation (press-fit), where the implant is designed to allow bone ingrowth
- A femoral head (metal or ceramic ball) is attached to the stem.
- The new ball-and-socket joint is reduced (repositioned), tested for stability, and the incision is closed.


Surgical Approaches for TKA
There are several approaches to accessing the hip joint, and the choice depends on surgeon preference, patient anatomy, and clinical factors:
- Posterior approach
The most commonly used technique. It provides excellent visibility of the joint but requires careful repair of soft tissues to reduce dislocation risk. - Anterior approach
A muscle-sparing technique that accesses the hip from the front. It may allow faster early recovery in some patients but requires specialized equipment and experience. - Lateral (anterolateral) approach
Accesses the hip from the side and offers good joint stability, but may involve partial detachment of hip abductor muscles.
Clinical Insight
Total hip arthroplasty (THA) is a standardized and highly effective surgical procedure in which the damaged hip joint is replaced with a prosthetic implant consisting of a femoral stem, femoral head, and acetabular cup.
Modern surgical techniques and implant designs provide reliable pain relief, restoration of mobility, and excellent long-term functional outcomes in appropriately selected patients.
Recovery After Total Hip Arthroplasty (THA)
Recovery after total hip arthroplasty (THA) is a structured, multi-phase process aimed at restoring mobility, strength, and independence while ensuring proper healing of the operated joint. Although recovery timelines may vary between individuals, most patients follow a predictable rehabilitation pathway.
1. Hospital Stay
Patients typically remain in hospital for a short period following surgery, usually between 2 and 5 days, depending on overall health status and postoperative progress.
During this phase:
- Pain is managed using a combination of analgesic medications and multimodal pain control strategies
- Early mobilization is initiated as soon as possible, often within 24 hours
- Patients are assisted to stand and begin walking with a walker or crutches
- Prevention of complications such as blood clots is a key priority
2. Early Rehabilitation Phase
Early rehabilitation begins immediately after surgery and continues during the first weeks at home.
Key goals include:
- Restoring safe mobility and basic independence
- Gradual improvement in hip range of motion
- Activation and strengthening of surrounding musculature (especially gluteal and quadriceps muscles)
- Gait training with assistive devices
During this phase, patients are instructed to avoid high-risk movements depending on surgical approach (e.g., extreme flexion or internal rotation).
3. Discharge and Functional Adaptation
After hospital discharge, patients may return home or transfer to a rehabilitation facility depending on individual needs.
Common recommendations include:
- Use of walking aids (crutches or walker)
- Home modifications to reduce fall risk
- Gradual return to daily activities such as dressing, bathing, and light household tasks
- Awareness of hip precautions to prevent dislocation
4. Structured Rehabilitation Program
Rehabilitation plays a crucial role in long-term success and can be delivered in different settings:
- Home-based physiotherapy
- Outpatient rehabilitation
- Inpatient rehabilitation in specialized facilities
Therapy focuses on:
- Progressive strengthening of hip and lower limb muscles
- Balance and proprioception training
- Improvement of walking pattern and endurance
5. Return to Daily Activities
Most patients return to basic daily activities within 6 to 12 weeks after surgery. Full recovery, including return to low-impact sports and more demanding activities, may take several months.
Long-term success depends on:
- Consistent rehabilitation
- Adherence to medical recommendations
- Gradual increase in physical activity
Clinical Insight
Recovery after total hip arthroplasty (THA) is a gradual but highly structured process that relies on early mobilization and a well-designed rehabilitation program.
With appropriate physiotherapy and good patient compliance, most individuals achieve significant pain relief, improved mobility, and a substantial improvement in overall quality of life.
Rehabilitation Phases (Overview)
| Phase | Timeframe | Key Goals |
|---|---|---|
| Hospital Phase | 0–5 days post-op | Pain control, early mobilization, prevention of complications |
| Early Rehabilitation | 1–3 weeks | Walking training, muscle activation, basic functional independence |
| Outpatient / Home Rehab | 3–12 weeks | Strengthening, balance training, gait normalization |
| Late Recovery Phase | 3–6+ months | Return to full function, low-impact sports, long-term conditioning |
Benefits and Risks of Total Hip Arthroplasty (THA)
Total hip arthroplasty (THA) is one of the most successful orthopedic procedures, providing substantial improvement in pain and function for patients with advanced hip joint disease. However, like all surgical interventions, it carries certain risks and potential complications.
Benefits of THA
- Significant pain reduction – most patients experience major or complete relief of chronic hip pain
- Improved mobility – restoration of joint function allows easier walking, climbing stairs, and daily activities
- Enhanced quality of life – increased independence and return to normal activities
- Improved sleep and comfort – reduction of night pain and stiffness
- Long-term durability – modern implants can last 15–25 years or longer in many patients
Potential Risks and Complications
Although complications are relatively uncommon, they can include:
- Infection – may occur early or late and sometimes requires revision surgery
- Dislocation of the prosthesis – especially in the early postoperative period
- Blood clots (deep vein thrombosis or pulmonary embolism)
- Leg length discrepancy – small differences in limb length may occur after surgery
- Implant loosening or wear over time – may require revision in the long term
- Nerve or vascular injury – rare but possible during surgery
- Persistent pain or stiffness – in a minority of patients despite technically successful surgery
Clinical Insight
Total hip arthroplasty (THA) is a highly effective procedure that provides significant pain relief, improved mobility, and substantial functional gains in patients with advanced hip joint disease.
Although outcomes are generally excellent, THA carries potential risks such as infection, dislocation, thromboembolic events, implant wear, and other procedure-related complications.
Careful patient selection, meticulous surgical technique, and structured rehabilitation are essential to minimize complications and optimize long-term results.
How Long Does a Hip Replacement Last?
Total hip arthroplasty (THA) implants are designed to provide long-term function and durability, but they are not considered lifetime devices for all patients. The lifespan of an artificial hip depends on multiple patient-related and implant-related factors.
Implant Longevity
Modern hip prostheses typically last 15 to 25 years, and in many cases even longer. Advances in materials, surgical techniques, and implant design have significantly improved long-term survival rates.
However, some patients may require revision surgery earlier, while others may never need a replacement revision in their lifetime.
Factors Affecting Implant Durability
Several key factors influence how long a hip replacement will last:
- Patient age and activity level – younger and more active patients tend to place higher mechanical stress on the implant
- Body weight and biomechanics – increased load can accelerate wear
- Implant type and materials – ceramic, polyethylene, and metal combinations differ in wear characteristics
- Surgical technique and implant positioning – accurate alignment improves longevity
- Bone quality – poor bone stock may affect fixation over time
- Comorbidities – conditions such as osteoporosis or inflammatory arthritis may influence outcomes
- Infection or complications – can significantly reduce implant survival
Clinical Insight
Modern total hip arthroplasty implants typically last 15–25 years or longer, with many patients achieving excellent long-term function without the need for revision surgery.
Implant longevity is influenced by multiple factors, including patient age, activity level, body weight, implant materials, surgical technique, and bone quality.
With optimal patient selection and precise surgical technique, THA provides durable pain relief and sustained functional improvement over decades.
Living After Total Hip Arthroplasty (THA)
After total hip arthroplasty (THA), most patients can return to an active and independent lifestyle. Long-term success depends on maintaining joint health, following activity recommendations, and avoiding movements that may increase the risk of complications.
Recommended Activities
Patients are encouraged to engage in low-impact activities that promote strength, mobility, and overall health, such as:
- Walking and gradual return to daily activities
- Cycling on a stationary or outdoor bike
- Swimming and water-based exercises
- Physiotherapy-guided strengthening and mobility exercises
- Light recreational activities such as golf or hiking (once fully recovered)
Regular physical activity helps maintain muscle strength and supports long-term implant function.
Activities to Avoid or Limit
Certain high-impact or risky activities should be avoided to reduce wear and the risk of complications:
- Running and high-impact sports (e.g., basketball, football)
- Jumping activities or repetitive heavy impact exercises
- Deep squatting or extreme hip flexion positions (especially early after surgery)
- High-risk activities with fall potential (contact sports, skiing in some cases)
Activity restrictions may vary depending on surgeon recommendations and implant type.
Long-Term Hip Care
Ongoing care is essential to ensure the longevity of the implant:
- Maintain a healthy body weight to reduce joint stress
- Continue regular strengthening and mobility exercises
- Attend scheduled follow-up appointments
- Be aware of any new pain, stiffness, or changes in function
- Use appropriate precautions during high-risk activities or travel
Clinical Insight
After total hip arthroplasty (THA), most patients can return to a highly functional and independent lifestyle, with significant improvements in pain, mobility, and overall quality of life.
Long-term success depends on engaging in low-impact activities, avoiding high-impact sports and extreme joint loading, and maintaining a healthy body weight.
Ongoing physiotherapy, regular follow-up, and awareness of joint health are essential to ensure long-term implant durability and optimal outcomes.
Frequently Asked Questions (FAQ)
How long does recovery take after THA?
Recovery after total hip arthroplasty typically takes 6 to 12 weeks for basic functional recovery, while full recovery and return to higher activity levels may take several months depending on the patient and rehabilitation progress.
Is hip replacement surgery painful?
The procedure itself is performed under anesthesia, so patients do not feel pain during surgery. Postoperative pain is expected in the early recovery phase, but it is well controlled with modern pain management strategies and gradually improves over time.
When can I walk after surgery?
Most patients begin walking within 24 hours after surgery with the help of a walker or crutches. Early mobilization is an important part of recovery and helps reduce complications.
How long does a hip replacement last?
Modern total hip arthroplasty implants typically last 15 to 25 years or longer, depending on factors such as activity level, implant type, surgical technique, and overall patient health.
Conclusion
Total hip arthroplasty (THA) is a highly effective surgical procedure for the treatment of advanced hip joint disease. It provides reliable pain relief, improved mobility, and restoration of function, significantly enhancing patients’ quality of life.
With modern implant designs, improved surgical techniques, and structured rehabilitation protocols, most patients achieve long-lasting and predictable outcomes. The overall goal of THA is not only to replace the damaged joint but also to enable patients to return to a more active, independent, and comfortable lifestyle.
American Academy of Orthopaedic Surgeons (AAOS). Total Hip Replacement. OrthoInfo. Available from: AAOS OrthoInfo
National Institute for Health and Care Excellence (NICE). Joint replacement (primary): hip, knee and shoulder. NICE Guideline [NG157]. Available from: NICE NG157
Goyal A, et al. Total Hip Arthroplasty. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025. Available from: NCBI StatPearls
American Association of Hip and Knee Surgeons (AAHKS). Hip Replacement Recovery and Expectations. Available from: AAHKS
National Health Service (NHS). Hip replacement – Recovery. Available from: NHS UK
Learmonth ID, Young C, Rorabeck C. The operation of the century: total hip replacement. Lancet. 2007;370(9597):1508–1519. doi:10.1016/S0140-6736(07)60457-7 PubMed
American Academy of Orthopaedic Surgeons (AAOS). Osteoarthritis of the Hip. Available from: AAOS OA Hip