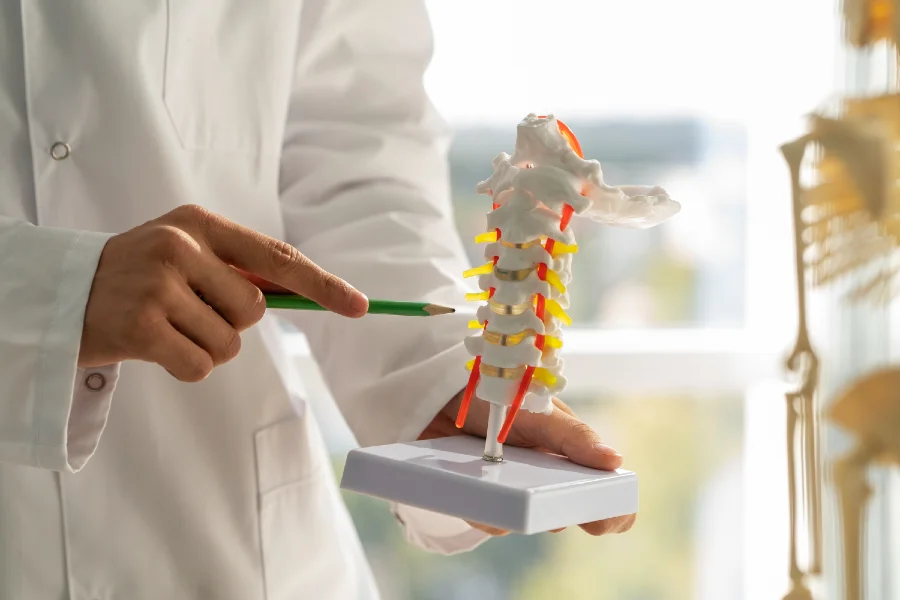
The cervical spine or C-spine is one of the most important and complex parts of the human skeletal system. It provides mobility of the head and protects the spinal cord, which enables the transmission of nerve signals between the brain and the rest of the body.
Although the cervical spine is anatomically designed to ensure both stability and mobility, due to its functional role and constant mechanical load it is particularly susceptible to various degenerative and functional changes. These changes may result in pain, stiffness, and difficulties in performing everyday activities.
In this article, you will learn about the cervical spine anatomy, its primary functions, and the most common symptoms, disorders, and conditions associated with this region of the spine.
Cervical Spine Anatomy
The cervical spine, medically referred to as the cervical vertebral column, consists of seven bones called cervical vertebrae, labeled C1 to C7. These vertebrae are stacked one on top of another like building blocks, forming a supportive column. The upper portion of the cervical spine connects to the skull, while the lower portion transitions into the upper thoracic spine at approximately shoulder level.
When viewed from the side, the cervical spine displays a natural inward curvature known as cervical lordosis, meaning it is gently curved backward like an arch. This curvature is essential for shock absorption, balance, and efficient head movement.
A common question is: how many cervical vertebrae in humans?
The answer is seven cervical vertebrae, a defining characteristic of the human spine.
Main Anatomical Components of the Cervical Spine
The cervical spine is composed of several key anatomical structures:
- Bones (7 cervical vertebrae)
- Facet joints
- Neck muscles
- Ligaments
- Spinal cord
- Nerve roots (spinal nerve roots or radices)
The letter “C” in the designation C1–C7 refers to the cervical region of the spine. Among these, the first (C1) and second (C2) cervical vertebrae are anatomically and functionally unique.
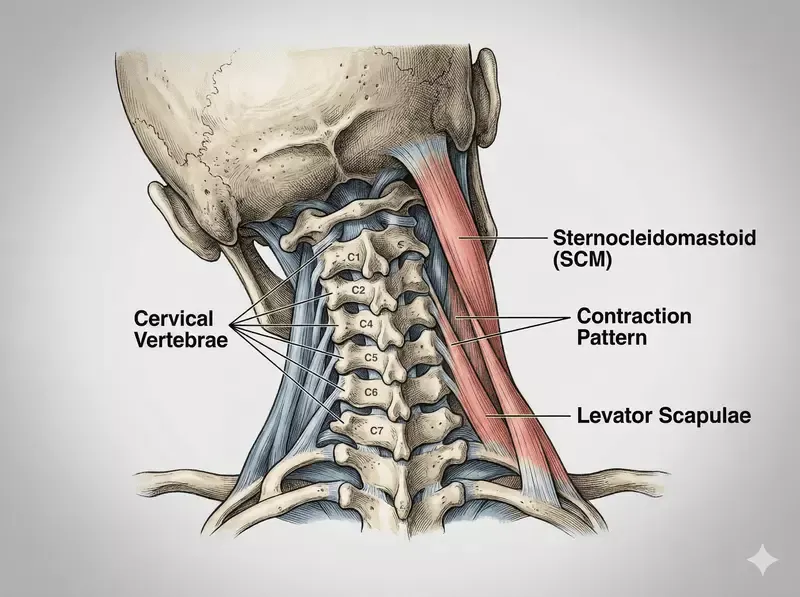
Atlas (C1) and Axis (C2)
The first cervical vertebra (C1), known as the atlas, is ring-shaped and sits directly at the base of the skull. It is named after Atlas from Greek mythology, who was said to carry the world on his shoulders. The atlas supports the skull and enables nodding movements of the head.
The second cervical vertebra (C2), called the axis, acts as a pivot. It allows the atlas—and therefore the head—to rotate from side to side, enabling the “no” movement of the head.
Joints, Muscles, and Intervertebral Discs
The seven cervical vertebrae (C1–C7) are connected posteriorly by paired facet joints, which allow flexion, extension, and rotational movements of the neck.
The cervical spine is surrounded by muscles, nerves, tendons, and ligaments that provide stability and control movement. Between most vertebrae are intervertebral discs, which function as shock absorbers and reduce mechanical stress during motion.
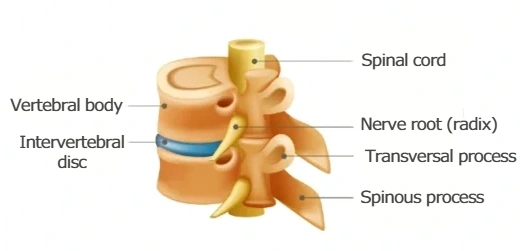
Running through the central spinal canal is the spinal cord, which transmits signals between the brain and the rest of the body and plays a critical role in controlling movement, sensation, and autonomic functions.
Spinal Cord and Cervical Nerve Roots
The spinal cord (medulla spinalis) serves as the main communication pathway between the brain and the body. In the cervical region, it is housed within a bony canal formed by the cervical vertebrae and is protected by three protective membranes (meninges) and cerebrospinal fluid, which provides additional cushioning against mechanical forces.
From the cervical spine emerge eight pairs of spinal nerves (C1–C8), despite the presence of only seven cervical vertebrae. These nerves exit between the vertebrae and branch out to different regions of the body, carrying:
- Motor (movement-related) signals
- Sensory (touch, pain, temperature) information
- Autonomic (vegetative) signals
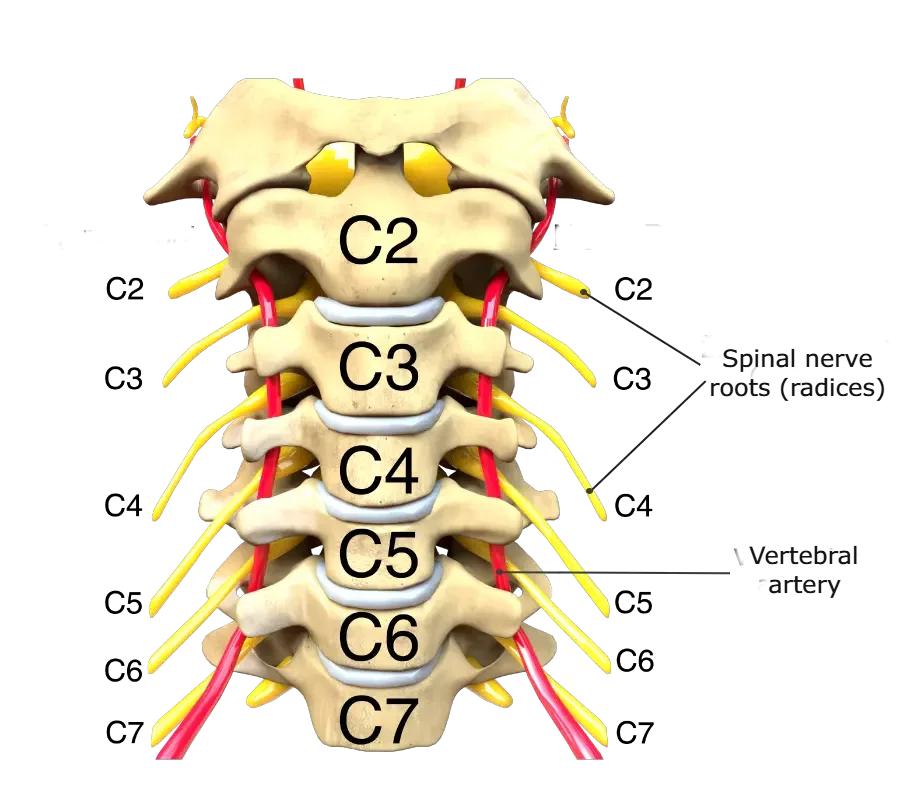
Each cervical nerve root controls specific muscles and transmits sensation from defined areas of the skin. For example:
- C1–C2: control head and neck movements
- C3: contributes to diaphragmatic function and breathing
- C5–C8: play a major role in controlling the arms, hands, and fingers, as well as sensation in the shoulders and upper limbs
Compression or damage to a cervical nerve root—such as from a herniated disc or bone spurs (osteophytes)—can lead to symptoms including neck pain radiating into the arm, tingling, muscle weakness, or sensory loss.
Clinical Importance:
It is important to note that severe injury to the spinal cord in the cervical region can result in serious neurological deficits, including partial or complete paralysis. This is because the cervical spine contains nerve pathways responsible for vital functions and for controlling all areas of the body below the level of injury.
Functions of the Cervical Spine
The cervical spine (cervical vertebral column) performs several essential functions, including:
- Protection of the Spinal Cord: The spinal cord is a bundle of nerves that extends from the brain and passes through the cervical and thoracic spine (upper and mid-back), ending just above the lumbar spine (lower back). Each vertebra contains a large opening called the vertebral foramen, through which the spinal cord passes. Together, all vertebrae form a bony tunnel known as the spinal canal, which effectively protects the spinal cord from external injury.
- Support of the Head and Facilitation of Movement: The cervical spine bears a significant mechanical load, as the average human head weighs between 4.5 and 6 kilograms. In addition to supporting the weight of the head, the cervical spine allows neck flexibility and a wide range of head movements, including bending forward and backward, rotation, and side bending.
- Enabling Blood Flow to the Brain: Small openings within the transverse processes of the cervical vertebrae serve as passageways for the vertebral arteries, which supply blood to the brain. These vascular openings are found exclusively in the cervical vertebrae from C1 to C6 (not in C7 or below).
Because many vital nerves, blood vessels, and joints are located within this relatively small anatomical region, the cervical spine is considered one of the most complex and functionally important parts of the human body.
Cervical Spine Symptoms: What Do Pain, Tingling, and Stiffness Mean?
Depending on the underlying cause, symptoms related to the cervical spine can vary significantly. By far, the most common symptoms are neck pain and neck stiffness, which are usually benign and not a cause for serious concern.
However, if there is irritation or injury to the spinal cord or to the nerves exiting the cervical spine, symptoms may include pain, numbness, or weakness radiating from the neck through the shoulders and down into the arms. This type of pain is known as radicular pain. Other possible symptoms can be more serious and are typically associated with damage to neural structures, including:
- Difficulty breathing due to paralysis of respiratory muscles
- Loss of normal bowel and bladder control, including constipation, incontinence, or bladder spasms
- Numbness
- Sensory changes
- Spasticity (excessive muscle tightness)
- Weakness or paralysis
In the following sections, the most common cervical spine–related symptoms are explained, along with their possible causes and underlying mechanisms.
1. Neck Pain

Neck pain is very common and, in most cases, not a reason for concern. It is often caused by muscle tension, such as after prolonged computer work, exposure to cold drafts, or sleeping in an awkward position. In many cases, the exact cause cannot be clearly identified.
Acute neck pain (often described as a “stiff neck” or “neck lock”) usually resolves within one to two weeks, although in some individuals it may recur in specific situations, such as intense physical exertion or work-related stress.
When symptoms persist for longer than three months, the condition is referred to as chronic neck pain, in which psychological stress often plays a significant role. Although many people avoid movement out of fear of worsening the pain, staying active is generally recommended. Light physical activity and targeted neck exercises can help prevent and alleviate symptoms.
2. Neck Stiffness
Neck stiffness commonly accompanies neck pain and restricts head movement, making everyday activities such as driving or working at a computer more difficult. In most cases, it is a harmless symptom.
The most frequent causes include muscle tension, poor posture, or sleeping in an improper position. Neck stiffness usually resolves spontaneously within a few days, especially with gentle stretching exercises and the application of heat. If stiffness persists or is accompanied by tingling in the arms, nerve irritation may be involved.
3. Neck and Shoulder Pain
Patients with neck pain often also report shoulder pain, which can sometimes pose a diagnostic challenge. The muscles of the upper back and neck function as a single biomechanical unit. When neck pain and muscle tension in the upper back are present, altered shoulder movement patterns may develop, leading to shoulder pain.
Degenerative changes and irritation of the cervical facet joints can also cause pain radiating to the neck and shoulder region. Additionally, irritation or compression of cervical nerve roots—particularly C5 and C6—may result in a burning pain that radiates from the neck toward the shoulder and shoulder blade.
4. Cervical Spine and Tingling in the Arms
Tingling in the arms is a relatively common symptom in individuals with neck pain, especially when symptoms are chronic. This can occur for two main reasons.
First, compression or irritation of a cervical nerve root (radix)—for example, due to a herniated disc or a bone spur (osteophyte), often referred to as “nerve inflammation in the neck”—can cause neck pain along with pain and tingling in the arm. The exact location of the tingling depends on which nerve is affected.
Second, tingling in the arms may represent referred sensations originating from overstrained and painful muscles around the shoulder blade and shoulder, commonly associated with myofascial trigger points.
If you experience tingling in your arms, it is recommended to read a dedicated article on this topic for further information.
5. Less Common Symptoms Associated with the Cervical Spine
In addition to pain and stiffness, degenerative changes or dysfunction of the cervical spine may cause a range of less well-known but highly uncomfortable symptoms that can significantly affect daily life. Circulatory disturbances, nerve compression, or muscle tension in this region may be associated with the following complaints:
- Dizziness and a sense of instability – The cervical spine can influence balance and cause dizziness, particularly during sudden head movements. Chronic neck muscle tension and degenerative changes of the facet joints are thought to play a role.
- Blurred vision – Neck pain may sometimes be accompanied by visual disturbances such as intermittent blurred vision. While often benign and related to muscle tension, these symptoms may also indicate more serious pathology.
- Facial tingling – Irritation of nerve structures may cause tingling or weakness in the facial region.
- Head tingling and tinnitus – Cervical spondylosis or muscle tension may lead to tingling in the back of the head, as well as ringing or buzzing in the ears.
- Pressure in the head – Many individuals with cervical spine disorders describe a feeling of pressure or heaviness in the head. Chronic neck pain is often associated with occipital headaches, which may spread from the back of the head toward the ear, forehead, and eye.
- Pulsation in the ear – Disturbances in blood flow through the cervical arteries are a rare cause of pulsating sensations in one or both ears.
These symptoms are not always a sign of a serious condition. However, if they persist or worsen over time, consultation with a healthcare professional is recommended for thorough evaluation and diagnosis.
Most Common Diagnoses Related to the Cervical Spine
The cervical spine is exposed to various mechanical stresses on a daily basis—from prolonged sitting at a computer and poor posture to aging and degenerative changes. For this reason, neck pain and cervical spine–related complaints are among the most common reasons for visiting a healthcare professional.
Some conditions are mild and temporary, such as muscle tension or strain, while others may require more detailed diagnostic evaluation and targeted treatment, including disc herniation or cervical spondylosis.
Below is an overview of the most common disorders and conditions affecting the cervical spine.
Most common cervical spine diagnoses:
1. Cervical Muscle Strain or Overuse
Cervical muscle strain or overuse is one of the most common causes of acute neck pain. It occurs when the neck muscles are exposed to excessive load, sudden movements, or prolonged static positions—for example, during long hours of computer work or sleeping in an improper position.
Symptoms include pain, stiffness, muscle tenderness to touch, and limited range of motion of the head and neck. In most cases, this condition is not serious and resolves spontaneously within a few days to a week with rest, gentle stretching, and the application of heat.
In more severe cases, headaches, dizziness, or pain radiating toward the shoulders may occur. Prevention includes regular neck-strengthening exercises, maintaining proper posture, and avoiding sudden movements or prolonged poor positioning.
2. Cervical Myofascial Pain Syndrome
Cervical myofascial pain syndrome is a common cause of persistent neck pain, particularly in women and middle-aged individuals. It develops due to the formation of so-called trigger points within muscles and fascia—the connective tissue surrounding muscles.
These trigger points are tender to pressure and may cause localized pain or referred pain to the head, shoulders, or arms. The pain is typically dull, persistent, and worsens with head movement or prolonged sitting, such as working at a computer.
The main contributing factors include poor posture, prolonged static muscle load, stress, and repetitive microtrauma. In addition to pain, patients may experience stiffness, reduced mobility, and tension-type headaches.
Treatment requires an individualized approach and may include physical therapy, massage, stretching exercises, and, when indicated, dry needling therapy. Prevention focuses on strengthening the neck muscles and maintaining proper posture during daily activities.
3. Cervical Spondylosis
Cervical spondylosis refers to degenerative changes affecting all structures of the cervical spine, including intervertebral discs, facet joints, uncovertebral (Luschka’s) joints, ligaments, and vertebral laminae. It is a natural age-related process that develops in most individuals after the age of 50.
Cervical spondylosis, also known as spinal osteoarthritis, is characterized by the formation of bony outgrowths called osteophytes (or spondylophytes). These changes may also be accompanied by disc degeneration, disc protrusion, disc herniation, or disc prolapse.
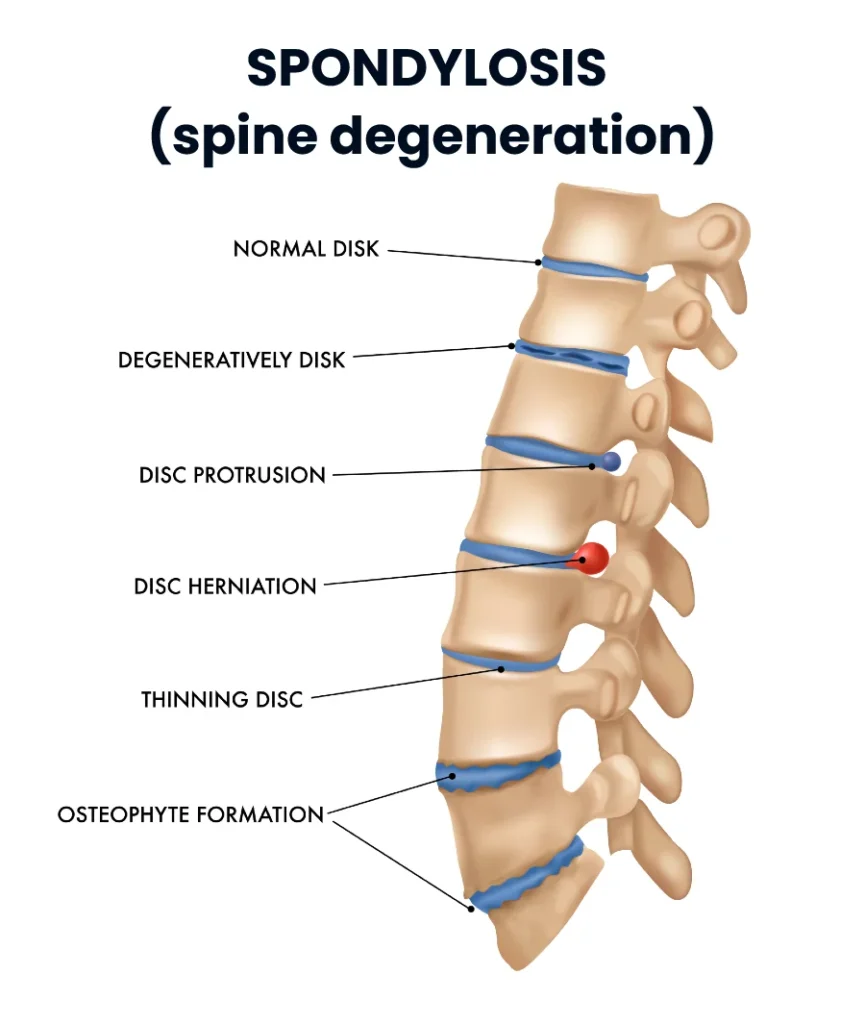
Despite visible degenerative changes on imaging, many people experience no symptoms. When symptoms occur, they most commonly present as neck pain and stiffness and may be accompanied by radicular symptoms if neural structures are compressed.
4. Cervical Radiculopathy
Cervical radiculopathy occurs when one or more nerve roots exiting the cervical spine are compressed or irritated. In younger patients, typically in their 30s and 40s, the most common cause is a herniated disc exerting pressure on a nerve root.
With increasing age, degenerative causes become more prevalent. Disc degeneration is the most common cause of radiculopathy in the fifth and sixth decades of life, while in the seventh decade, osteophytes and spondylophytes that narrow the neural foramina (foraminal stenosis) are the leading cause.
The main symptoms of cervical radiculopathy include pain radiating from the neck into the shoulder, arm, and fingers, tingling in the arms, weakness, or sensory loss in the affected areas. Pain may worsen with neck movements, especially rotation or side bending, but in some cases may persist throughout the day regardless of movement.
Diagnosis is based on clinical examination and imaging studies, most commonly MRI or CT. Treatment includes physical therapy, analgesics, anti-inflammatory medications, and, in more severe cases, surgical intervention.
5. Cervical Spinal Canal Stenosis and Cervical Myelopathy
Cervical spinal canal stenosis is a condition characterized by narrowing of the space through which the spinal cord and nerve roots pass. This narrowing may result from degenerative changes such as osteophyte formation, thickening of ligaments, or herniation of intervertebral discs.
Spinal canal stenosis can compress neural structures, leading to symptoms such as neck pain, tingling and weakness in the arms, and disturbances in sensation and coordination.
When the narrowing is severe and compresses the spinal cord itself, cervical myelopathy develops. This condition is associated with more serious neurological symptoms, including weakness in the legs, difficulty walking, loss of fine motor control in the hands, sensory deficits, and problems with bladder or bowel control.
Cervical myelopathy requires prompt and accurate diagnosis, as untreated cases may lead to permanent neurological damage. Treatment depends on the severity of stenosis and symptoms and may include physical therapy, medication, or surgical decompression of the spinal canal.
Frequently Asked Questions About the Cervical Spine
1. When is neck pain a reason for concern?
Neck pain is most often not a cause for concern and usually resolves within a few days to two weeks. Even if the pain lasts longer—several weeks or even months—and becomes chronic, it is still most commonly not related to a serious condition. However, regardless of the cause, chronic neck pain can significantly affect quality of life.
Urgent medical evaluation is required if neck pain is accompanied by symptoms such as tingling or weakness in the arms, loss of bladder or bowel control, dizziness, or breathing difficulties. Additionally, neck pain that occurs after an injury or fall should always be assessed promptly.
2. How can cervical radiculopathy be recognized?
Cervical radiculopathy occurs when a nerve root in the cervical spine is compressed or irritated. The main symptoms include pain radiating from the neck into the shoulder, arm, and fingers, as well as tingling, numbness, or weakness in the affected arm.
The pain often worsens with head movements, particularly rotation or side bending. If you experience these symptoms, it is recommended to consult a healthcare professional for proper diagnosis and treatment.
3. How can cervical spine problems be prevented?
Prevention of cervical spine problems includes maintaining proper posture, avoiding prolonged static positions, and performing regular strengthening and stretching exercises for the neck muscles. It is also important to pay attention to workplace ergonomics, use appropriate head and neck support during sleep, and stay physically active throughout the day.
Stress can contribute to increased muscle tension, so relaxation techniques and stress management strategies can also play an important preventive role.
4. What is cervical spondylosis and is it a cause for concern?
Cervical spondylosis is a degenerative, age-related process affecting the cervical spine, including the intervertebral discs, joints, and ligaments. During this process, bony outgrowths (osteophytes) may form on the vertebrae, facet joints degenerate, joint spaces narrow, and joint cartilage gradually wears down.
Intervertebral discs also undergo degeneration—they lose fluid content and height, their structure changes, the outer annulus may develop fissures, and disc protrusions can occur.
Cervical spondylosis is a natural process that develops to a greater or lesser extent in all individuals as they age and often causes no symptoms at all. Therefore, if your doctor mentions cervical spondylosis or it appears on an X-ray report, it is generally not a reason for alarm.
Rahman S, Das JM. Anatomy, Head and Neck: Cervical Spine. [Updated 2023 Aug 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK557516/
https://www.spine-health.com/conditions/spine-anatomy/cervical-vertebrae
InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Overview: Neck pain. [Updated 2022 Dec 12]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK338120/
Cohen SP. Epidemiology, diagnosis, and treatment of neck pain. Mayo Clin Proc. 2015 Feb;90(2):284-99. doi: 10.1016/j.mayocp.2014.09.008. PMID: 25659245.
Touma J, May T, Isaacson AC. Cervical Myofascial Pain. [Updated 2023 Jul 3]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK507825/
Kuo DT, Tadi P. Cervical Spondylosis. [Updated 2023 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK551557/
Magnus W, Viswanath O, Viswanathan VK, et al. Cervical Radiculopathy. [Updated 2024 Jan 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK441828/
https://www.physio-pedia.com/Structure_and_Function_of_the_Cervical_Spine
Morishita Y, Naito M, Wang JC. Cervical spinal canal stenosis: the differences between stenosis at the lower cervical and multiple segment levels. Int Orthop. 2011 Oct;35(10):1517-22. doi: 10.1007/s00264-010-1169-3. Epub 2010 Nov 27. PMID: 21113592; PMCID: PMC3174302.
Donnally III CJ, Hanna A, Odom CK. Cervical Myelopathy. [Updated 2023 Jan 15]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482312/