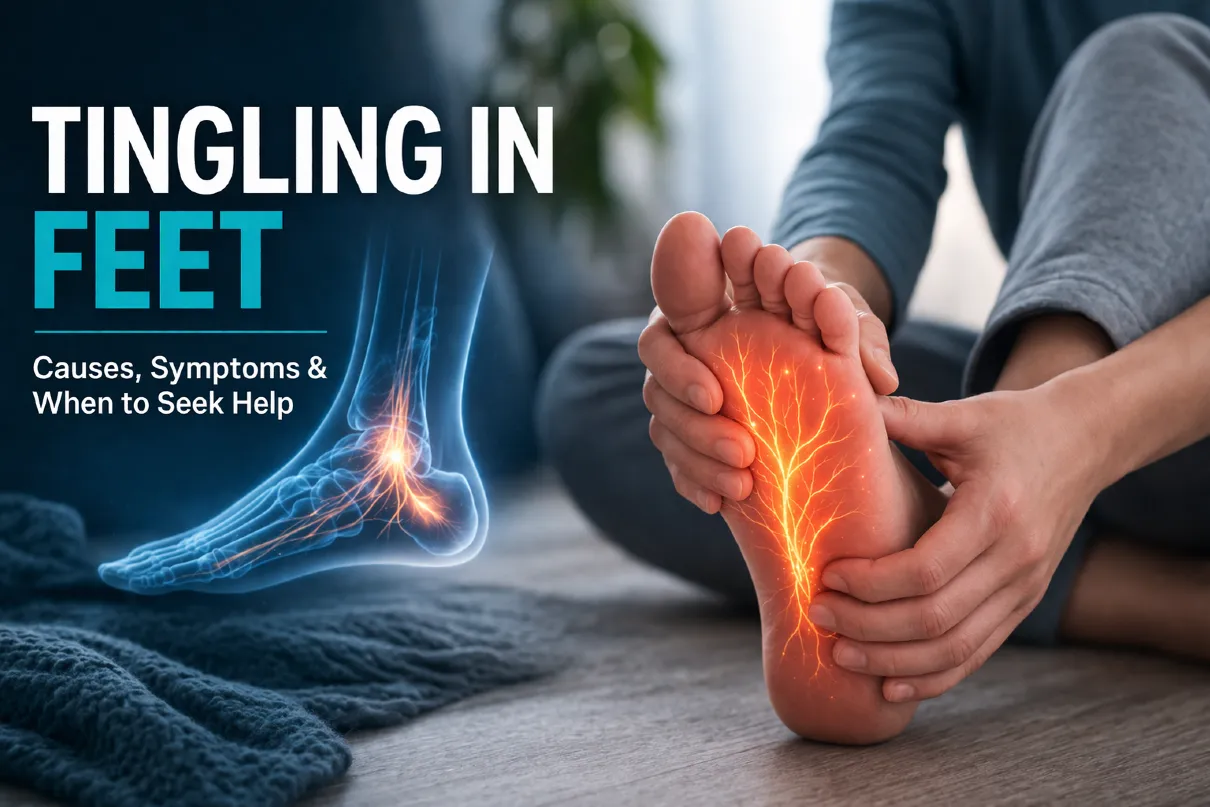
Neuropathy in feet is a common yet often misunderstood condition that can significantly affect quality of life. As a physician working with musculoskeletal and nerve-related conditions, I frequently see patients describing symptoms such as tingling in feet, pins and needles in feet, or a persistent burning sensation in legs.
These symptoms are typically caused by damage or dysfunction of peripheral nerves and may gradually worsen if left unaddressed. In many cases, neuropathy in legs develops alongside underlying conditions such as diabetes, nerve compression, or circulatory issues.
Recognizing early signs of foot neuropathy is essential for preventing progression and improving long-term outcomes.
In this guide, I’ll explain what neuropathy in feet feels like, the most common medical causes, and evidence-based strategies that can help relieve symptoms and support nerve health.
What Is Neuropathy in Feet?
Neuropathy in feet refers to damage or dysfunction of the peripheral nerves that carry sensory and motor signals between the brain, spinal cord, and the lower extremities. These nerves are essential for normal sensation, balance, and coordination.
When nerve function is impaired, patients may develop a range of symptoms commonly described as tingling in feet, pins and needles in feet, or a persistent burning sensation in legs. In more advanced stages, foot neuropathy can lead to numbness and reduced protective sensation, increasing the risk of unnoticed injuries.
Clinically, neuropathy in feet is not a single disease but a symptom of underlying nerve damage. The condition may result from metabolic disorders such as diabetes, mechanical nerve compression, nutritional deficiencies, or systemic neurological conditions.
A key feature of peripheral neuropathy is its typical progression. Symptoms often begin in the feet and gradually spread upward, leading to what is referred to as neuropathy in legs. This pattern, sometimes described as a “stocking distribution,” is highly relevant in clinical assessment and diagnosis.
From a medical standpoint, early identification of neuropathy in feet is critical. Prompt evaluation allows clinicians to identify the underlying cause, initiate appropriate management, and reduce the risk of long-term complications.
Symptoms of Neuropathy in Feet
Neuropathy in feet can present with a wide range of sensory symptoms, which often develop gradually and may worsen over time. The severity and pattern of symptoms depend on the extent and type of nerve involvement.
The most common early symptom is tingling in feet, often described as a mild “pins and needles” sensation. This feeling may come and go initially but can become more persistent as nerve damage progresses. Many patients also report a burning sensation in legs or feet, which can be particularly noticeable at night.
As the condition advances, symptoms of foot neuropathy may include:
- Persistent tingling in feet that does not resolve with movement
- Pins and needles in feet that become more intense or frequent
- Burning sensation in legs, especially during rest or at night
- Numbness or reduced ability to feel touch, temperature, or pain
- Sharp, stabbing, or electric-like pain in the feet
- Increased sensitivity to touch (even light pressure may feel painful)
In more severe cases, neuropathy in feet can affect proprioception and balance. Patients may feel unsteady while walking or have difficulty sensing the position of their feet, increasing the risk of falls.
Another important clinical feature is the distribution of symptoms. Neuropathy typically follows a symmetrical pattern, affecting both feet and sometimes progressing upward into the lower legs, which is often referred to as neuropathy in legs.
From a medical perspective, the progression from mild sensory changes to more pronounced symptoms highlights the importance of early recognition. Identifying symptoms of neuropathy in feet at an early stage allows for timely intervention and may help slow or prevent further nerve damage.
What Causes Neuropathy in Feet?
Neuropathy in feet can develop due to a variety of underlying conditions that damage or impair peripheral nerves. Understanding what causes neuropathy in feet is essential for effective treatment, as the condition is often a symptom rather than a standalone diagnosis.
The most common causes of foot neuropathy include:
Diabetes (Diabetic Neuropathy)
Diabetes is the leading cause of neuropathy in feet. Chronically elevated blood glucose levels can damage small blood vessels that supply nerves, leading to progressive nerve dysfunction. Diabetic neuropathy typically presents as symmetrical symptoms starting in the feet and may progress to neuropathy in legs over time.
Nerve Compression and Spinal Issues
Mechanical compression of nerves, particularly in the lower spine, can lead to symptoms in the feet. Conditions such as lumbar disc herniation or spinal stenosis may irritate or compress nerve roots, resulting in tingling in feet, numbness, or a burning sensation in legs.
Vitamin Deficiencies
Deficiencies in essential nutrients, especially vitamin B12, can impair nerve function. Vitamin-related neuropathy often develops gradually and may present with pins and needles in feet, weakness, and sensory changes.
Alcohol and Toxins
Chronic alcohol consumption is a well-known cause of peripheral neuropathy. Alcohol-related nerve damage can lead to persistent tingling in feet, burning pain, and progressive sensory loss. Exposure to certain toxins or heavy metals may produce similar effects.
Medications
Some medications, particularly certain chemotherapy agents and long-term use of specific drugs, can cause nerve damage. Medication-induced neuropathy may present with symptoms similar to other forms of foot neuropathy, including numbness and altered sensation.
Inflammatory and Autoimmune Conditions
Conditions such as autoimmune neuropathies or systemic inflammatory disorders can affect peripheral nerves. These cases may progress more rapidly and often require specialized medical evaluation.
Idiopathic Neuropathy
In some patients, no clear cause can be identified despite thorough evaluation. This is referred to as idiopathic neuropathy and is relatively common, especially in older adults.
From a clinical standpoint, identifying what causes neuropathy in feet is crucial because treatment strategies depend on addressing the underlying condition. Early diagnosis and targeted management can significantly reduce symptoms and help prevent progression of nerve damage.
From a clinical perspective, understanding the underlying causes of neuropathy in feet is essential. The table below summarizes the most common etiologies and their characteristic features.
| Cause | Description | Typical Features |
|---|---|---|
| Diabetic neuropathy | Nerve damage caused by prolonged high blood glucose levels affecting small blood vessels and nerve fibers. | Symmetrical symptoms, starts in feet, burning, numbness, gradual progression |
| Lumbar radiculopathy | Compression or irritation of nerve roots in the lower spine due to disc herniation or degeneration. | Radiating leg pain, possible tingling in feet, often unilateral, associated with back pain |
| Vitamin B12 deficiency | Insufficient vitamin B12 leading to impaired nerve function and myelin damage. | Pins and needles in feet, fatigue, balance issues, possible cognitive symptoms |
| Alcohol-related neuropathy | Peripheral nerve damage due to chronic alcohol use and associated nutritional deficiencies. | Symmetrical tingling in feet, burning sensation in legs, weakness, slow progression |
| Medication-induced neuropathy | Nerve damage caused by certain medications, including some chemotherapy agents. | Numbness, tingling in feet, symptoms related to medication timing |
| Peripheral polyneuropathy | Diffuse damage affecting multiple peripheral nerves, often due to systemic conditions. | Symmetrical symptoms, distal onset in feet, sensory loss, progression to legs |
| Tarsal tunnel syndrome | Compression of the tibial nerve as it passes through the tarsal tunnel near the ankle. | Burning pain in sole, tingling in foot, worse with standing or walking |
| Peripheral artery disease | Reduced blood flow to the lower limbs due to arterial narrowing. | Cold feet, pain while walking, reduced pulses, possible tingling |
| Idiopathic neuropathy | Neuropathy with no clearly identifiable cause despite evaluation. | Gradual onset, often mild but persistent symptoms, common in older adults |
Neuropathy in Feet vs Neuropathy in Legs
Neuropathy in feet and neuropathy in legs are closely related conditions that typically represent different stages or distributions of the same underlying nerve dysfunction. In most cases, symptoms begin in the feet due to the longer nerve fibers being more vulnerable to damage, and then gradually progress upward into the lower legs in a characteristic “stocking” pattern.
Neuropathy in feet usually presents first with localized sensory symptoms such as tingling in feet, pins and needles in feet, or a burning sensation in legs focused around the feet and toes. At this early stage, symptoms may be intermittent and mild, often worse at night.
As the condition progresses, neuropathy in legs becomes more apparent. Symptoms extend upward from the feet into the calves and may include increased numbness, reduced sensation, and impaired balance. This progression reflects more extensive peripheral nerve involvement.
From a clinical perspective, the distinction between neuropathy in feet and neuropathy in legs is important because it helps determine the stage and potential cause of nerve damage. Recognizing the pattern of spread also assists in differentiating peripheral neuropathy from localized nerve entrapment syndromes, guiding further diagnostic evaluation and treatment strategy.
Clinical Insight
In clinical practice, neuropathy in feet often represents the earliest stage of a length-dependent peripheral neuropathy, with symptoms gradually progressing upward into the lower legs over time.
This distal-to-proximal pattern is highly characteristic and helps differentiate peripheral neuropathy from more localized nerve entrapment syndromes.
When Should You Be Concerned?
Neuropathy in feet is often a slowly progressive condition, but certain symptoms may indicate a more serious underlying problem and should not be ignored.
You should be particularly concerned if symptoms begin to worsen rapidly over a short period of time, as this may suggest an active or progressive nerve injury. The development of muscle weakness in the feet or lower legs is another important red flag, especially if it affects walking or daily activities.
Loss of balance or coordination is also clinically significant, as it may indicate more advanced nerve involvement affecting proprioception. Patients may notice increased unsteadiness, frequent tripping, or difficulty walking in the dark.
Medical attention should be sought promptly if these symptoms appear, or if neuropathy in feet is accompanied by new neurological signs such as severe pain, asymmetry of symptoms, or sudden changes in sensation. Early evaluation allows for identification of potentially reversible causes and helps prevent further progression into neuropathy in legs or more widespread nerve dysfunction.
Diagnosis: How Doctors Identify Foot Neuropathy
The diagnosis of neuropathy in feet begins with a structured clinical assessment. Physicians first take a detailed medical history focusing on symptom onset, progression, and associated risk factors such as diabetes, alcohol use, medication exposure, or nutritional deficiencies. This step is essential because neuropathy in feet is a symptom rather than a single disease entity.
A focused neurological examination is then performed to assess sensory function, reflexes, muscle strength, and balance. These findings help determine the extent and pattern of nerve involvement and whether the presentation is consistent with peripheral neuropathy.
To confirm the diagnosis and assess severity, several diagnostic tests may be used:
- Nerve conduction studies (NCS): Evaluate how efficiently electrical signals travel through peripheral nerves and help classify the type of nerve damage.
- Blood tests: Identify underlying causes such as diabetes, vitamin B12 deficiency, thyroid dysfunction, or systemic inflammation.
- Additional investigations: In selected cases, imaging such as MRI may be used if nerve compression or spinal pathology is suspected.
A crucial part of the diagnostic process is differential diagnosis, since symptoms like tingling in feet, pins and needles in feet, or a burning sensation in legs can also occur in vascular disease, radiculopathy, or musculoskeletal disorders.
Accurate differentiation is essential for appropriate treatment planning and to prevent progression of neuropathy in legs or more generalized nerve dysfunction.
Treatment Options for Neuropathy in Feet
The treatment for neuropathy in feet depends primarily on identifying and managing the underlying cause, as neuropathy in feet is a symptom rather than a single disease. A targeted approach is essential for achieving symptom relief and preventing further progression of nerve damage.
Treat the Underlying Cause
The most important step in the treatment for neuropathy in feet is addressing the root cause. In patients with diabetes, improved blood glucose control is crucial to slow or prevent further nerve damage. If neuropathy is related to vitamin deficiencies, such as vitamin B12 deficiency, correction of the deficiency can significantly improve symptoms. In cases related to alcohol use, reducing or stopping alcohol intake is essential. When nerve compression or spinal pathology is present, treatment is directed toward relieving mechanical pressure on the affected nerves.
Medications
Pharmacological treatment for neuropathy in feet is mainly focused on symptom control rather than reversing nerve damage. Certain medications may be used to reduce neuropathic pain, burning sensation in legs, and discomfort associated with tingling in feet or pins and needles in feet. These medications are selected based on symptom severity and patient tolerance, and are typically used when conservative measures are not sufficient.
Physical Therapy and Movement
Physical therapy plays an important role in maintaining function and improving quality of life. Structured exercises can help improve balance, strength, and coordination, especially in patients with neuropathy in legs. Regular movement also supports circulation and may help reduce symptom severity over time. In some cases, targeted rehabilitation programs are recommended to reduce fall risk and improve gait stability.
Lifestyle Changes
Lifestyle modification is an essential part of the treatment for neuropathy in feet. Patients are often advised to maintain a healthy weight, engage in regular low-impact physical activity, and ensure adequate nutritional intake. Proper foot care is also important to prevent complications, especially in patients with reduced sensation. Avoiding alcohol and managing chronic conditions can further help stabilize symptoms and slow progression.
A combined approach that addresses the underlying cause, supports nerve health, and manages symptoms provides the best outcomes for patients with neuropathy in feet (also referred to as foot neuropathy).
Home Remedies and Daily Tips for Neuropathy in Feet
Managing neuropathy in feet at home focuses on supporting nerve function, improving circulation, and reducing symptom severity in daily life. While these strategies do not treat the underlying cause, they can significantly improve comfort and quality of life when used consistently.
Regular low-impact exercises are highly beneficial. Activities such as walking, gentle stretching, or stationary cycling help maintain muscle strength, improve balance, and stimulate blood flow to the lower extremities. This is particularly important in patients experiencing neuropathy in legs, where reduced activity can worsen stiffness and instability.
Improving circulation is another key aspect of symptom management. Elevating the feet when resting, avoiding prolonged sitting, and incorporating light movement throughout the day can help reduce tingling in feet and discomfort. Some patients also benefit from gentle foot massages, which may temporarily relieve sensations such as pins and needles in feet.
Proper footwear is essential. Shoes should provide adequate support, cushioning, and enough space to avoid pressure on sensitive areas. Poorly fitted shoes can worsen symptoms and increase the risk of injury in patients with reduced sensation due to foot neuropathy.
Establishing a consistent daily routine can also help stabilize symptoms. This includes regular physical activity, good sleep hygiene, foot inspection, and avoiding triggers such as prolonged pressure or inactivity. Over time, these habits can help reduce symptom fluctuations and improve overall nerve health support.
Can Neuropathy in Feet Be Reversed?
Whether neuropathy in feet can be reversed depends primarily on the underlying cause, the severity of nerve damage, and how early the condition is diagnosed. In many cases, neuropathy is not fully reversible, but symptoms can often be significantly improved or stabilized with appropriate treatment.
If the condition is identified early, there is a greater chance of improvement, especially when the underlying cause is treatable. For example, neuropathy related to vitamin B12 deficiency or poor blood glucose control may improve once the deficiency is corrected or diabetes is better managed. In these cases, nerve function can partially recover over time.
In more advanced stages, where prolonged nerve damage has occurred, full reversal is less likely. However, even in chronic neuropathy in legs or feet, symptom progression can often be slowed, and quality of life can be improved with targeted management strategies.
From a clinical perspective, early diagnosis and intervention remain the most important factors in determining outcomes. The earlier neuropathy in feet is recognized and treated, the higher the likelihood of meaningful recovery or long-term symptom control.
FAQ: Neuropathy in Feet
Can neuropathy in feet go away?
Neuropathy in feet may improve depending on the underlying cause. If the condition is identified early and the cause is treatable, such as vitamin B12 deficiency or poorly controlled diabetes, symptoms can partially improve or stabilize. However, in more advanced cases of nerve damage, complete reversal is less likely.
What is the best treatment for foot neuropathy?
The most effective treatment for neuropathy in feet focuses on addressing the underlying cause. This may include improving blood sugar control in diabetes, correcting nutritional deficiencies, reducing alcohol intake, or treating nerve compression. Symptom management, physical therapy, and lifestyle changes also play an important role in improving function and reducing discomfort.
Why do my feet tingle at night?
Tingling in feet at night is a common symptom of neuropathy in feet. It often becomes more noticeable during rest because there are fewer distractions and changes in circulation or nerve sensitivity may make symptoms more apparent.
Is walking good for neuropathy?
Yes, in most cases walking is beneficial for neuropathy in feet. Regular low-impact walking helps improve circulation, maintain muscle strength, and support nerve health. However, intensity should be adjusted based on symptoms, especially if neuropathy in legs affects balance or stability.
Conclusion
Neuropathy in feet is a complex condition that can significantly affect daily function, comfort, and quality of life. It often begins subtly with symptoms such as tingling in feet, pins and needles in feet, or a burning sensation in legs, and may gradually progress if the underlying cause is not identified and managed.
From a clinical perspective, early recognition and proper evaluation are essential, as neuropathy in feet is usually a manifestation of an underlying condition rather than an isolated disease. Understanding the cause allows for more targeted treatment and better long-term outcomes.
While complete reversal is not always possible, many patients experience meaningful improvement with appropriate management, especially when intervention occurs early. Lifestyle changes, medical treatment, and supportive therapies can all contribute to symptom control and functional improvement.
Mayo Clinic Staff. Peripheral neuropathy – Symptoms and causes. Mayo Clinic. Available from: Mayo Clinic
National Institute of Neurological Disorders and Stroke (NINDS). Peripheral Neuropathy Fact Sheet. NIH. NINDS NIH
Cleveland Clinic. Peripheral Neuropathy: Symptoms, Causes & Treatment. Cleveland Clinic
NHS (UK). Peripheral neuropathy overview. NHS
American Diabetes Association. Diabetic neuropathy complications. ADA
Johns Hopkins Medicine. Peripheral Neuropathy Overview. Johns Hopkins Medicine
Harvard Health Publishing. Peripheral neuropathy causes and symptoms. Harvard Health
MedlinePlus (U.S. National Library of Medicine). Peripheral neuropathy. MedlinePlus
National Institute on Aging (NIA). Nerve damage and neuropathy. NIA
World Health Organization (WHO). Diabetes complications overview. WHO
BMJ Best Practice. Peripheral neuropathy clinical overview. BMJ Best Practice